Atsushi Hamuro1, Minoru Honda2, Yuya Wakaura2, Shouko Mori3, Ryuichi Tanaka4
1. Yuzuriha Hospital, Department of Psychiatry, Nagasaki City, Japan; 2. Yuzuriha Hospital, Department of Nursing, Nagasaki City, Japan; 3. Yuzuriha Hospital, Department of Nutrition, Nagasaki City, Japan; 4. Yuzuriha Hospital, Department of Dentistry, Nagasaki City, Japan
Corresponding to: Atsushi Hamuro, 413 Sanwamachi, Nagasaki City, Nagasakiken 850-0975, Japan. Tel: +81-95-878-3734; Fax: +81-95-878-3289. E-mail: ahamuro007@yahoo.co.jp
Care Weekly 2020;4:8-10
Published online December 10, 2020, http://dx.doi.org/10.14283/cw.2020.2
Abstract
We investigated the effect of mousse meals on improvement in nutritional status. We conducted a 12-week, prospective, structured clinical trial on 11 elderly patients with psychiatric disorders. We compared the participants’ body mass index, blood protein and albumin levels, activities of daily living, and swallowing function, as well as presence of pneumonia, urinary-tract infection, and incidences of gastrointestinal symptoms due to consumption of mousse meals during the baseline and 12-week follow up. Results showed that Body Mass Index levels significantly increased, while blood protein and albumin levels, activities of daily living, and swallow function varied. One patient with pneumonia and another with urinary-tract infection could resume eating mousse meals within one week from the onset of infection. No participant suffered from gastrointestinal symptoms. The results of this study indicate that mousse meals are a viable choice for improving low nutritional status of elderly patients with psychiatric disorders.
Keywords: Mousse meal, Low nutrition, Psychiatric disorder.
Introduction
In many countries, including Japan, life expectancy is growing. As a result, the elderly among the population (above 65 years) are increasing (1). Nutritional issues are important as the nutritional status among the elderly tends to be lower (2). However, nutritional issues have received little attention in geriatric psychiatry research (3).
Some of the factors that cause low nutritional status in elderly patients with psychiatric disorders include health complications (e.g., hypertension, heart disorder, and diabetes), gastrointestinal disorders (e.g., constipation, ileus, and diarrhea), malignant tumors, infections, and worsening psychiatric symptoms (4). Moreover, other studies considered inadequate meal forms as its cause (e.g., soft food, mixer food) (5). Thus, we investigated the effects of special food, i.e., mousse meals, considering the adhesion, cohesion, and hardness of food such as jelly, on the improvement of nutritional status.
Methods
Study Design
This study was 12-week, prospective, structured clinical trial.
Participants
Of the patients (N = 319) who were hospitalized at the Department of Psychiatry in Yuzuriha Hospital, we enrolled a total of 11 hospitalized patients (four females and seven males; mean age: 78.73±10.9) with psychiatric disorders (Alzheimer’s disease = 3, vascular dementia = 3, schizophrenia = 1, and mental retardation = 4) on October 2017, which serves as the point of baseline. Their psychiatric disorders were diagnosed according to the criteria of the International Classification of Diseases, Tenth Revision (ICD-10). We excluded those on general meals (N = 127), soft meals (N = 171), and mixed meals (N = 10). All the patients required assistance while eating. Moreover, we used Global Assessment of Functioning (GAF) (6) to compute for the scale-defined psychological function (ranging from 0 to 100, with lower scores indicating increased severity of psychological function) of our patients, resulting in an average score of 30.
Interventions
Patients’ medications related to the treatment of their psychiatric disorders were not changed during the study period. The criteria for providing mousse meals were as follows: patients had to (1) store food in their mouth without swallowing, (2) experience loss of appetite, and (3) exhibit the presence of dysphagia, as determined by the Nutrition Dysphagia Rehabilitation Committee of Yuzuriha Hospital. Body mass index (BMI), blood protein and albumin levels, activities of daily living (ADL), and swallowing function, as well as the presence of pneumonia, urinary-tract infection, and incidences of gastrointestinal symptoms due to the consumption of the mousse meal were compared at the baseline and 12-week follow up. The mousse meals comprised a total energy of 1400 Kcal (protein = 42.1g, lipid = 35.2g, and carbohydrate = 210.7g) per day. ADL and swallowing function were evaluated using the Physical Self-Maintenance Scale (PSMS) (7), and the scale based on the Japanese Society of Dysphagia Rehabilitation (8). The scale assesses sitting in an upright posture, palsy, pronunciation, lip protrusion, tongue movement, and pharyngeal reflex, with scores for each item ranging from 0 to 3, where higher scores mean enhanced swallowing function normality.
Data Analysis
Statistical differences between all scores were determined using the Wilcoxon signed rank test. P values of <0.05 were considered to be statistically significant.
Results
All the patients completed the study. Table 1 shows the comparison and scores at baseline and at 12 weeks for all the patients. Only BMI level was significantly associated between the baseline and at 12 weeks. The levels of blood protein and albumin, scales of ADL, and swallow function did not significantly increase. During the study, there was one patient with pneumonia and another with urinary-tract infection. No patient suffered from gastrointestinal symptoms such as stomachache, vomiting, constipation, ileus, or diarrhea.
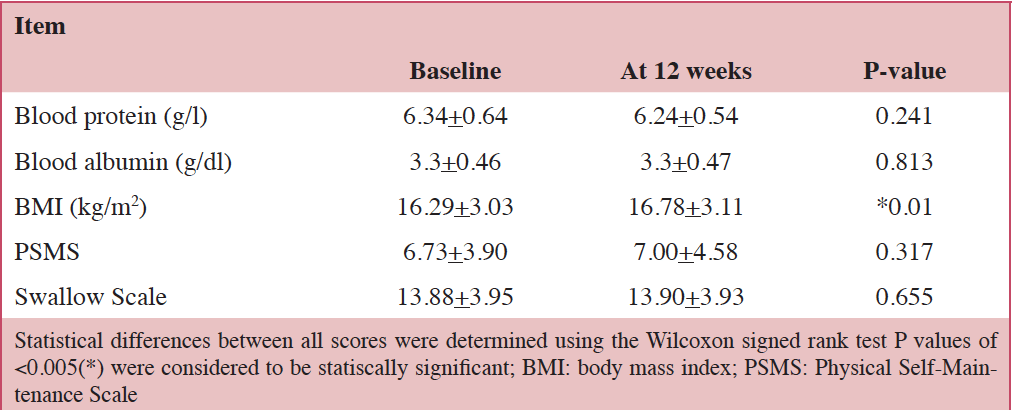
Table 1. Mean scores for blood protein, albumin, BMI, PSMS, and swallowing scale in the 11 elderly patients with psychiatric disorders
Statistical differences between all scores were determined using the Wilcoxon signed rank test P values of <0.005(*) were considered to be statiscally significant; BMI: body mass index; PSMS: Physical Self-Maintenance Scale
Discussion
Patients with psychiatric disorders and low GAF scores often react poorly (e.g., they do not open their mouths or store food in them) when receiving assistance to eat a meal (9, 10). As a result, poor nutrition is common in elderly hospitalized patients with psychiatric disorders (11). Previous studies have been conducted to determine the relationship between falls, infection, mortality, and nutritional risks (12, 13). However, to our knowledge, few studies involving elderly patients with psychiatric disorders have described the relationship between low nutritional status and special food forms, such as mousse meals. Therefore, we sought to determine which meal form is most suitable to the conditions of elderly hospitalized patients with psychiatric disorders. As blended meals, with several ingredients mixed in a mixer, do not collect in the mouth, swallowing function often worsens. Moreover, it is difficult to determine the ingredients of blended meals. On the other hand, mousse meals, which grind only one ingredient (e.g., meat, fish, vegetable) and add thicker liquids address this problem, given that they are portioned in a suitable bolus outside the mouth and their ingredients are clearly visible.
Although the BMI levels of patients showed a significant increase, they are still unsatisfactory as per the BMI defined in Japan (14).The levels of blood protein and albumin varied during the study since they may take a little longer to increase. There was no negative impact on ADL and swallowing function. Patients with pneumonia and urinary-tract infection were completely cured within one week from the onset of infection, thus, the mousse meal was resumed. The patients did not present any gastrointestinal symptoms after consuming the mousse meal.
The limitations of this study include the small number of patients and lack of reliability and validity testing. However, we were able to increase staff awareness about the food forms they could provide to hospitalized patients with psychiatric disorders. Such awareness is as important as nursing homes and care centers in the community.
The results of this study indicate that mousse meals are a viable choice for improving the low nutritional status of elderly patients with psychiatric disorders. Further studies are needed to explore the relationship between mousse meals and improvement in low nutritional status, while also considering the meal forms and observation of complications, oral care, swallowing function, and psychiatric symptoms in the future.
Funding
This study received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Acknowledgments
The authors wish to thank Mamiko Shimada, Mayumi Yamasaki, and Junko Kamito for the help in following up with patients in the present study.
Conflicts of Interest
The authors declare no conflicts of interest.
Ethical standards
The Yuzuriha Hospital Ethics Committee approved the safeguards, protocols, and informed consent procedure of the study in according with the declaration of Helsinki. After explaining the study to the patients and caregivers, written informed consent was obtained from all the patients.
References
1. Trinh NT, Bernard NR, Ahmed II. Mental health issues in racial and ethnic minority elderly. Curr Psychiatry Rep. 2019;14 (21):102.
2. Pilgrim LA, Robinson MS, Sayer AA, Roberts CH. An overview of appetite decline in older people. Nurs Older People. 2015;27 (5):29–35.
3. Bhat RS, Chiu E, Jeste DV. Nutrition and geriatric psychiatry: A neglected field. Curr Opin Psychiatry. 2005;18 (6):609–614.
4. Suzuki Y, Mikami T, Tajiri M. Effects of hospitalization in a psychiatric ward on the body weight of Japanese patients with schizophrenia. Int J Psychiatry Med. 2013;45 (3):261–268.
5. Chen TB, Weng SC, Chou YY. Predictors of mortality in the oldest old patients with newly diagnosed Alzheimer disease in a residential aged care facility. Dement Geriatr Cogn Disord. 2019;48 (1-2):93–104.
6. Hall RC. Global assessment of functioning. A modified scale. Psychosomatics. 1995;36 (3):267–275.
7. Lawton MP, Brody EM. Assessment of older people: Self-maintaining and instrumental activities of daily living. Gerontologist. 1969;9(3_Part_1):179–186.
8. Ueda K, Okada S, Kitasumi E, Koyama T, Takahashi K, Takehara I, et al. The dysphagia scale (the simplified version), the JSDR dysphagia diet committee. Jpn Soc Dysphagia Rehabil. 2011;15:96–101.
9. Jablonski RA, Kolanowski A, Therrien B, Mahoney EK, Kassab C, Leslie DL. Reducing care-resistant behaviors during oral hygiene in persons with dementia. BMC Oral Health. 2011;19:11–30.
10. Bertaud GV, Kovess MV, Perrus C, Trohel G, Richard F. Oral health status and treatment needs among psychiatric inpatients in Rennes, France: A cross-sectional study. BMC Psychiatry. 2013;21:227.
11. Molteno C, Smit I, Mills J, Huskisson J. Nutritional status of patients in a long-stay hospital for people with mental handicap. S Afr Med J. 2000;90 (11):1135–1140.
12. Yoshinaga N, Baba T, Koga T. Evaluation of the texture of food for the dysphagia diet served in hospital. Int Univ Rev. 2017;17:199–209.
13. Tsai MT, Chang TH, Wu BJ. Prognostic impact of nutritional risk assessment in patients with chronic schizophrenia. Schizophr Res. 2018;192:137–141.
14. Araki A, Yokote K, Ito H, Rakugi H, Yamamoto K, Arai H, et al. Elderly obesity guideline (2018) Japanese Journal of Geriatrics. 2018;55:464–538, (in Japanese).
