JULIE M. ROBILLARD1,2, EMANUEL CABRAL1, TANYA L. FENG1
1. Division of Neurology, Department of Medicine, The University of British Columbia, Vancouver, BC, Canada
2. BC Children’s and Women’s Hospital, Vancouver, BC, Canada
Corresponding to: JM Robillard, PhD, Scientist, Children’s and Women’s Hospital and Health Centres, Assistant Professor of Neurology, The University of British Columbia, B402 Shaughnessy, BC Children’s and Women’s Hospital, 4480 Oak Street, Vancouver, BC V6H 3N1 Canada, [T] 604-875-3697, [F] 604-822-0361, [E] jrobilla@mail.ubc.ca
Care Weekly 2018;2:14-20
Published online November 5, 2018, http://dx.doi.org/10.14283/cw.2018.8
Abstract
Background: Online health information-seeking is a common behavior among caregivers. Social media increasingly plays a role as a source of health information, including for novel or emerging treatments such as deep-brain stimulation.
Objectives: To examine health information-seeking related to deep brain stimulation.
Design: Content analysis was applied to questions and answers related to deep brain stimulation posted online.
Setting: Content was captured from the website Yahoo! Answers between 2006 and 2015.
Participants: No participants were recruited for this study. The analysis was conducted on freely-accessible publicly posted content in online social media.
Results: Most discussions involved information-seeking and -sharing about a disease, treatment, or the procedure for deep brain stimulation. Nearly half of the questions featured some emotional valence, most often negative. Only a minority of questions and answers mentioned risks associated with deep brain stimulation. Deep brain stimulation was most discussed in the context of age-associated movement disorders such as Parkinson disease. Evaluations of the benefits and efficacy of deep brain stimulation for movement disorders differed significantly from evaluations of its use for mental health disorders (X2 [6, N = 432] = 28.46, p < 0.01).
Conclusions: With the increasing use of deep brain stimulation and its expanding application to a variety of age-associated neurological and psychiatric conditions, it is crucial to understand information-seeking trends related to this emerging neurotechnology to inform the development of knowledge dissemination initiatives for the public, patient and caregivers, and heath care providers.
Key words: Deep brain stimulation, social media, Parkinson’s disease, aging, eHealth.
Introduction
Over half of online health information-seekers are doing so on behalf of a person they care for (1). As the information needs of caregivers are not always met through formal health care channels, online resources and social media are increasingly used as sources of health information. Online health information-seeking may be especially relevant for new or emerging interventions, as analyses of social media content from our group and the work of others shows extensive discussions on topics such as gene therapy, stem cells, and optogenetics (2–6). One such intervention is deep brain stimulation (DBS), which is increasingly viewed as a novel neuro-technology with tremendous potential to alleviate symptoms and suffering from a large number of conditions. While one of the primary clinical indications is the treatment of advanced Parkinson’s disease, it has also been approved by the Food and Drug Administration for essential tremor and has humanitarian device exceptions for obsessive-compulsive disorder and dystonia (7). Ongoing research continues to explore applications of DBS for a wide spectrum of other neurological and psychiatric conditions. Clinical trials have shown efficacy for several diseases and disorders to date, including depression, Alzheimer’s disease, and chronic pain (8), many of which are especially relevant for an aging population.
Despite the rapidly expanding applications of DBS, little research has been conducted to examine information-seeking related to this type of intervention. Research specifically investigating perspectives on DBS is scarce and where attitudes have been evaluated, much of the literature has focused primarily on clinician and surgeon opinions (9), patient or research participant attitudes (10, 11), or media portrayals (12). The limited research available on public attitudes and information-seeking towards DBS has highlighted some of the ethical issues contemplated by individuals who have undergone or might undergo DBS. Pervasive themes of risk versus benefit, informed consent and autonomy underlie patient discussions and decision-making. Leykin et al. found that clinical trial participants considering DBS for treatment-resistant depression demonstrated a reasonable awareness of the risks and benefits of the procedure, weighing the risks of an unproven procedure against the harm of remaining clinically depressed (11). Analysis of interviews with patients with Parkinson’s disease who had underdone DBS showed that patients considered the procedure in different ways based on the level of knowledge acquired through the media, the internet, advocacy societies, or friends (13).
The media plays a pervasive role in shaping public opinions and attitudes and can be an important influence on views and behaviours related to health (14). With regards to DBS specifically, content analyses of news reports on neuro-stimulation and DBS treatments have identified predominant themes such as hope and scientific breakthrough (12). As a result, some researchers have expressed concern that overly optimistic media portrayals of DBS may harm informed consent and have suggested that both journalists and scientists should be more careful to include discussion on ethical issues, including greater exposition of the risks and potential limitations when communicating about DBS (15, 16).
In addition to traditional media, social media is used with increasing frequency as a means to both disseminate and access health information and to increase interactions between patients, care providers and researchers (17). Previous research has shown that social media platforms such as Twitter and Yahoo! Answers provide a rich resource for examining the health information being shared by the public and public attitudes, including views towards novel biotechnologies (2, 3, 18). Question-and-answer (Q&A) platforms in particular can yield rich insights into information needs, and attitudes and opinions towards emerging health technologies, as users with varying levels of expertise can both ask and answer questions on a topic. Yahoo! Answers is one of the most popular Q&A forums, with 661 million visits in November, 2017 (19). On this social media platform, users post questions for other members of the community to answer. A Best Answer is selected for each question by either the asker or the community. Categories of discussion vary from society and culture to politics and government and everything in between, and include thousands of health-specific threads.
Investigations of online health conversations about DBS can help elucidate public perspectives and attitudes toward to this novel treatment with expanding applications to several neurological and psychiatric diseases. These perspectives and attitudes can in turn serve as a critical starting point to inform the development of knowledge dissemination initiatives for the public, and for patients and their caregivers. The goal of the present study is to examine information-seeking and discussions of DBS through a content analysis of questions and answers on Yahoo! Answers.
Methods
Sample
A customized, automatic data mining program was used to collect Yahoo! Answers threads using the keywords “deep brain stimulation”, “brain pacemaker”, “brain surgery”, “brain electrode”, and “psychosurgery” across a 10-year period from 2006 to 2015. A thread is defined here as a question and its associated answers. Duplicates were manually removed in cases where different keywords retrieved identical threads. Where a question was posted multiple times and elicited different answers, identical questions were removed and unique answers were collected under a single thread. In order to select for DBS-relevant threads, we only included those that referenced “electrode in the brain” or in a specific deep brain region, “deep brain stimulation” or “DBS”, either in the questions or in their respective answers. Threads that did not discuss DBS for human applications were removed. Questions in the final sample were categorized into discreet and mutually exclusive question types.
To extract a sample of answers with entries focused on DBS, answers were collected from a subsample of questions that were categorized into question types where DBS was mentioned in greater than 10% of the questions. Answers that did not mention DBS and were not answering a question that mentioned DBS were removed to produce the final sample of answers (Appendix 1).
Content analysis
Questions
Emergent coding was employed to develop the coding guide for analysis of the questions, based on a pilot analysis of a random 10% of the sample conducted independently by two coders (JMR and EC) to capture salient themes. The final coding guide was developed through discussion (Appendix 2). The unit of analysis was each individual question or answer. A rich coding strategy was employed, allowing for each question or answer to be categorized into multiple codes. The entire question sample was coded by EC, and TF coded 20% of the sample in order to determine inter-coder reliability. Agreement was initially 95% and disagreements were resolved through discussion.
Answers
The same coding guide development process was repeated for the answers (Appendix 3). The entire answer sample was coded by one researcher (EC) and a second researcher (TF) coded 35% of the sample. After an iterative process of comparing coding results and refining the coding guide, a final agreement of 92% was obtained. Remaining differences were resolved through discussion.
Results
Sample
A total of 4860 questions were retrieved using the keywords and 776 questions remained after duplicates were removed. Of these, 645 questions met the inclusion criteria and comprised the final sample for analysis.
Questions
The questions were sorted into the following 13 categories (Appendix 2): application, opinion, information-sharing, access, health advice, information-seeking about procedure, information-seeking about disease, information-seeking about treatment, information-seeking about charity or financial coverage, homework, and experience.
Answers
DBS was mentioned in greater than 10% of questions in the access, application, health advice, homework, experience and information-seeking categories, therefore answers from these 480 questions were collected to form the initial answers sample. Of those questions, 3980 answers that did not mention DBS and were not answering a question that mentioned DBS were removed, resulting in the final answers for analysis (Na = 556).
Content analysis
Questions
The final coding guide comprised the following major themes (Appendix 2): 1) type of question; 2) for whom the question was being asked; 3) emotions expressed in the question; 4) features of DBS; 5) and the impact of illness. Half of all questions (50%, 325/645) specifically requested factual information such as information about diseases (15%, 98/645), treatments (14%, 92/645), or details about a specific procedure (10%, 62/645). In contrast, a different subset of questions asked about or expressed opinions on various subjects (12%, 79/645). While most questions did not explicitly state who the question was for (68%, 436/645), some Yahoo! Answers users mentioned that the question was for an issue that they were personally dealing with (21%, 135/645) or that a family member or friend was dealing with (11%, 74/645).
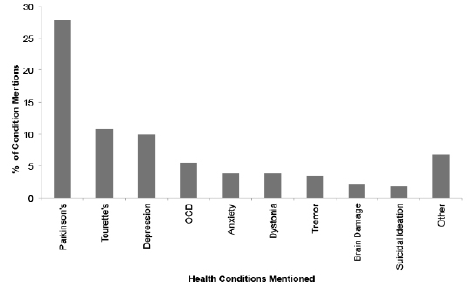
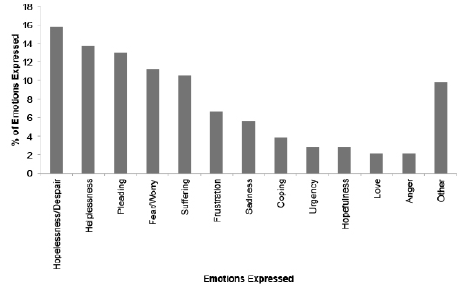
Among the health conditions mentioned (Figure 1), Parkinson’s disease was mentioned most frequently (28%, 152/543), followed by Tourette syndrome (11%. 59/543) and depression (10%, 54/543). Among the questions with specific mention of the impact of a health condition (n = 151), the main themes were impact on mobility (36%, 55/151), daily activities (31%, 47/151), social isolation (14%, 21/151), work (11%, 17/151) and school (7%, 11/151). Emotions were expressed in 285 questions, sometimes with multiple emotions expressed within the same question (Figure 2). Among these emotions, questions expressed a lack of hope or despair (16%, 45/285), a perceived lack of control or helplessness (14%, 39/285), and pleas for help or information (13%, 37/285).
Various features of DBS were discussed, sometimes within the same question, for a total of 203 mentions (n = 203). This included identifying the use of an electrode (37%, 76/203) and describing the device as a type of pacemaker (5%, 11/203). There was also some mention of risk involved in the procedure (9%, 18/203) and discussion of the use of DBS in children (6%, 13/203).
Answers
The final coding guide for the answers included the following final themes (Appendix 3): 1) type of response; 2) features of DBS; 3) evaluations of DBS. Among the types of answers, there was sharing of information about treatments (48%, 268/556), medical procedures (27%, 152/556) and diseases (24%, 131/556). Some answers used personal experience or personal information (21%, 116/556) to emphasize their point while others provided advice about how to proceed on a medical issue (19%, 106/556; Figure 5).
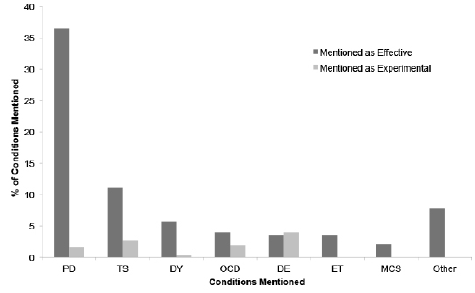
Figure 3: Frequency of conditions mentioned among all health conditions referenced in the answers as compared between disorders for which DBS was mentioned as effective and for which DBS was mentioned as an experimental treatment (PD: Parkinson disease; TS: Tourette syndrome; DY: dystonia; OCD: obsessive-compulsive disorder; DE: depression; ET: essential tremor; MCS: minimally conscious state)
There were several mentions of conditions that were discussed as targets of DBS (n = 480). Mainly, DBS was mentioned as effective for Parkinson’s disease (36%, 175/480), Tourette syndrome (11%, 53/480) and dystonia (6%, 27/480; Figure 3). We categorized all conditions mentioned in our samples into two separate disease types: movement disorders or mental health disorders based on whether they primarily affect mobility or psychiatric well-being, respectively. The movement disorders category included: Parkinson’s disease, Tourette syndrome, dystonia, minimally conscious state, and essential tremor, while the mental health disorders category included obsessive compulsive disorder and depression. Across these categories, most mentions of conditions described DBS as an effective treatment for movement disorders (64%, 308/480) and some of these mentions described DBS as an effective treatment for mental health disorders (9%, 44/480). We compared whether risk was brought up for these categories of disorders (Figure 4). Overall 19% (90/480) of disease mentions included some discussion of risk, with 20% (72/359) of movement disorder mentions containing discussion of risk and 16% (23/144) of mental health disorder mentions containing discussion of risk. Using a chi-squared analysis, we compared the distributions of risk mentions across the mental health and movement disorder categories, and found no significant difference, X2 (1, N = 480) = 1.12, p = .29.
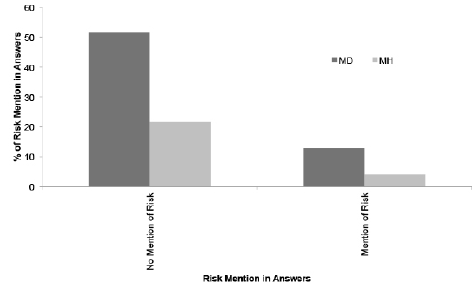
Figure 4: Mention of risk among all answers (N=556) compared between answers mentioning movement disorders (MD) and answers mentioning mental health disorders (MH)
We also compared how answers evaluated DBS and compared these evaluations to the disease types that were mentioned in conjunction with these evaluations (Figure 5). Overall, there were 359 evaluations (n = 359), of which 24% (85/359) described DBS as a last resort, 23% (81/359) described it as an option to consider, and 21% (76/359) expressed some reservation about the procedure. Our chi-squared analysis showed a significant difference between the distribution for the evaluation of DBS among movement disorders when compared to the distribution for the evaluation of DBS among mental health disorders, X2 (6, N = 432) = 28.46, p < 0.01.
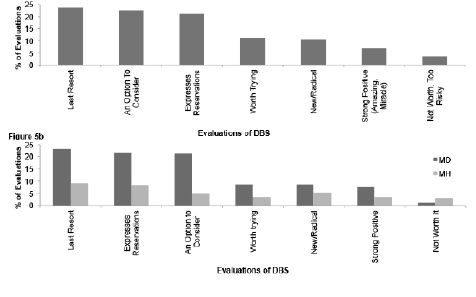
Figure 5: a. Evaluations of DBS among all answers; b. Evaluation of DBS among all answers referencing disease, compared between movement disorders (MD) and mental health disorders (MH)
Discussion
Our study builds on previous understanding of public attitudes towards novel medical treatments by examining public information-seeking and opinions towards DBS. Most discussions examined here involved the seeking and sharing of information about a disease, treatment, or procedure for DBS, with minimal discussions of risk in both questions and answers.
In general, DBS was more likely to be discussed in the context of movement disorders than mental health disorders. Furthermore, the distribution of the evaluation of DBS of movement disorders significantly differed from that of mental health disorders. Some questions also mentioned the impact of the condition such as on mobility, daily activities, and social isolation. In addition, almost half of the questions featured some emotional valence, most commonly negative, such as a lack of hope or a perceived lack of control or helplessness.
The predominance of movement disorders over mental health disorders in this analysis may be attributed to the history of clinical applications of DBS, as modern DBS was first used in the treatment of movement disorders and has only more recently been applied to treating psychiatric disorders (7). These circumstances may contribute to less public awareness of the use of DBS in the treatment of mental illnesses, but as research advances, public knowledge of these novel applications may increase.
The differing evaluations of DBS between its use in movement disorders and mental health disorders may be the result of several sociocultural factors. One possible explanation is the mainstream understanding of the self according to the naturalistic notion of personality. Synofzik and Schaepler (20) argue that if we define personality as a “continuum where cognitive and mood representations are complex representations that largely build on more basic sensorimotor and vegetative representations”, DBS for any indication may be perceived to affect personality. However, this alteration of the self is the primary intended outcome of DBS for psychiatric disorders and is necessary for clinical benefit. Perhaps it is this fundamental and unavoidable change in psychiatric applications of DBS that some may find more ethically problematic than the use of DBS for movement disorders. Another explanation for this discrepancy may be the lasting impact of “the troubled history of psychosurgery” (21), namely, the widespread use of lobotomy to treat mental illness, on the public’s perception of DBS.
The paucity of discussion of the risks of DBS parallels the findings of Racine and colleagues in their examination of media portrayals of neurostimulation techniques, as they found that the tone of this coverage was generally optimistic and focused on the benefits of the technology (12). This has implications for raising unrealistic expectations of the benefits of DBS, which may be especially concerning in the present situation given the significant impact of these illnesses and the related themes of hopelessness and despair. This may also have an impact on shaping individuals’ provisional opinions on DBS, which Kimmerle and colleagues demonstrated may subsequently affect how people perceive further information about DBS (22).
As DBS continues to expand in its clinical applications, public views on this neuro-technology will be informed by the information disseminated through various sources, including social media platforms such as Yahoo! Answers as well as traditional media. The scientific community has already called for the responsible reporting of DBS in the media (23), including discussion of its associated ethical issues (15). However, this burden does not fall on the shoulders of journalists alone, as Illes et al. call for greater engagement between neuroscientists and the public in order to improve neuroscience communication and public understanding of the brain (24). This cultural shift is already underway, as a recent analysis of optogenetics-related tweets on Twitter found that academic researchers constituted the largest group involved in the conversation (4). This may be one of the contributing factors to the generally neutral tone of the tweets, compared to discussions of other biotechnologies on Twitter (3).
Public understanding of DBS has critical health implications on the individual scale, such as influencing informed consent and patient and caregiver expectations, as well as a broader societal scale such as determining its acceptance (25). Bell and colleagues (25) also emphasize the potential benefits of increased awareness of DBS, including increased funding and decreased stigma surrounding the treatment and the conditions it is used to treat.
We appreciate the limitations of the present study. While Yahoo! Answers is a popular social media website, future work should examine discussions about DBS taking place on other social media platforms. In addition, due to the anonymity of the users, we cannot conclude that these findings are generalizable to the broader population. Also, although our sample captures threads from a comprehensive 10-year period contributing to the stability of the sample, we did not conduct analyses to determine if and how information-seeking and perspectives on DBS changed over time.
Despite these limitations, this study provides a window into public understanding and perspectives on DBS. With the combination of the lack of discussion on the dangers of the procedure and its current and potential applications to several debilitating conditions, involvement of both the media and the academic community is crucial to ensure an accurate understanding of the benefits and risks of DBS.
Funding
This study was funded by the Canadian Institutes for Health Research, the Foundation for Ethics and Technology, the Vancouver Coastal Research Institute and the BC Children’s Hospital Foundation. The sponsors had no role in the design and conduct of the study; in the collection, analysis, and interpretation of data; in the preparation of the manuscript; or in the review or approval of the manuscript.
Conflict of Interest
None.
References
1. Sadasivam RS, Kinney RL, Lemon SC, Shimada SL, Allison JJ, Houston TK. Internet health information seeking is a team sport: Analysis of the Pew Internet Survey. Int J Med Inf. 2013 Mar 1;82(3):193–200.
2. Robillard JM, Whiteley L, Johnson TW, Lim J, Wasserman WW, Illes J. Utilizing Social Media to Study Information-Seeking and Ethical Issues in Gene Therapy. J Med Internet Res [Internet]. 2013 Mar 4;15(3). Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3636301/
3. Robillard JM, Cabral E, Hennessey C, Kwon BK, Illes J. Fueling Hope: Stem Cells in Social Media. Stem Cell Rev. 2015 Aug;11(4):540–6.
4. Robillard JM, Lo C, Feng TL, Hennessey CA. “A Light Switch in the #Brain”: Optogenetics on Social Media. Neuroethics. 2016 Dec 1;9(3):279–88.
5. Scanfeld D, Scanfeld V, Larson EL. Dissemination of health information through social networks: twitter and antibiotics. Am J Infect Control. 2010 Apr;38(3):182–8.
6. Paige SR, Stellefson M, Chaney BH, Alber JM. Pinterest as a Resource for Health Information on Chronic Obstructive Pulmonary Disease (COPD): A Social Media Content Analysis. Am J Health Educ. 2015 Jul 4;46(4):241–51.
7. Miocinovic S, Somayajula S, Chitnis S, Vitek JL. History, applications, and mechanisms of deep brain stimulation. JAMA Neurol. 2013 Feb;70(2):163–71.
8. Lyons MK. Deep brain stimulation: current and future clinical applications. Mayo Clin Proc. 2011 Jul;86(7):662–72.
9. Dijkstra AM, Schuijff M. Public opinions about human enhancement can enhance the expert-only debate: a review study. Public Underst Sci Bristol Engl. 2016;25(5):588–602.
10. Hamberg K, Hariz G-M. The decision-making process leading to deep brain stimulation in men and women with parkinson’s disease – an interview study. BMC Neurol. 2014 Apr 25;14:89.
11. Leykin Y, Christopher PP, Holtzheimer PE, Appelbaum PS, Mayberg HS, Lisanby SH, et al. Participants’ perceptions of deep brain stimulation research for treatment-resistant depression: risks, benefits, and therapeutic misconception. AJOB Prim Res. 2011 Oct 1;2(4):33–41.
12. Racine E, Waldman S, Palmour N, Risse D, Illes J. “Currents of hope” : Neurostimulation Techniques in U.S. and U.K. Print Media. Camb Q Healthc Ethics. 2007 Jul;16(03):312–6.
13. Hamberg K, Hariz G-M. The decision-making process leading to deep brain stimulation in men and women with parkinson’s disease – an interview study. BMC Neurol. 2014;14:89.
14. Grilli R, Ramsay C, Minozzi S. Mass media interventions: effects on health services utilisation. Cochrane Database Syst Rev. 2002;(1):CD000389.
15. Gilbert F, Ovadia D. Deep brain stimulation in the media: over-optimistic portrayals call for a new strategy involving journalists and scientists in ethical debates. Front Integr Neurosci. 2011;5:16.
16. Schlaepfer TE, Lisanby SH, Pallanti S. Separating hope from hype: some ethical implications of the development of deep brain stimulation in psychiatric research and treatment. CNS Spectr. 2010 May;15(5):285–7.
17. Moorhead SA, Hazlett DE, Harrison L, Carroll JK, Irwin A, Hoving C. A new dimension of health care: systematic review of the uses, benefits, and limitations of social media for health communication. J Med Internet Res. 2013 Apr 23;15(4):e85.
18. Robillard JM, Johnson TW, Hennessey C, Beattie BL, Illes J. Aging 2.0: health information about dementia on Twitter. PLoS ONE. 2013;8(7):e69861.
19. Answers.yahoo.com Analytics – Market Share Stats & Traffic Ranking [Internet]. [cited 2017 Dec 16]. Available from: https://www.similarweb.com/website/answers.yahoo.com
20. Synofzik M, Schlaepfer TE. Stimulating personality: ethical criteria for deep brain stimulation in psychiatric patients and for enhancement purposes. Biotechnol J. 2008 Dec;3(12):1511–20.
21. Rabins P, Appleby BS, Brandt J, DeLong MR, Dunn LB, Gabriëls L, et al. Scientific and Ethical Issues Related to Deep Brain Stimulation for Disorders of Mood, Behavior, and Thought. Arch Gen Psychiatry. 2009 Sep 1;66(9):931–7.
22. Kimmerle J, Flemming D, Feinkohl I, Cress U. How Laypeople Understand the Tentativeness of Medical Research News in the Media: An Experimental Study on the Perception of Information About Deep Brain Stimulation. Sci Commun. 2015 Apr 1;37(2):173–89.
23. Cleary DR, Ozpinar A, Raslan AM, Ko AL. Deep brain stimulation for psychiatric disorders: where we are now. Neurosurg Focus. 2015 Jun 1;38(6):E2.
24. Illes J, Moser MA, McCormick JB, Racine E, Blakeslee S, Caplan A, et al. Neurotalk: improving the communication of neuroscience research. Nat Rev Neurosci. 2010;11(1):61–9.
25. Bell E, Mathieu G, Racine E. Preparing the ethical future of deep brain stimulation. Surg Neurol. 2009 Dec 1;72(6):577–86.