L. Neumann1, U. Dapp1, W. Von Renteln-Kruse1, C.E. Minder2
1. Albertinen-Haus, Geriatrics Centre, Scientific Department at the University of Hamburg, Hamburg, Germany; 2. Horten-Zentrum, University of Zürich, Postfach Nord, Zürich, Switzerland.
Corresponding to: Lilli Neumann, Albertinen-Haus, Geriatrics Centre, Scientific Department at the University of Hamburg, Sellhopsweg 18-22, D-22459 Hamburg, Germany, Tel.: ++49-40-5581-1692; Fax: ++49-40-5581-1874; E-Mail: lilli.neumann@albertinen.de
Care Weekly 2017;1:21-30
Published online November 9, 2017, http://dx.doi.org/10.14283/cw.2017.6
Please, note that this editorial was published also in the Journal of the Nutrition Healh and Aging (JNHA) https://link.springer.com/article/10.1007/s12603-017-0932-1
Abstract
Objectives: An RCT of a health promotion and preventive care intervention was done in 2001-2002. Here, long-term analyses based on 12 years of follow-up of survival and of change in functional competence between intervention and control group are presented. Positive 1-year results (significantly higher use of preventive services and better health behaviour) were presented earlier.
Design: Parallel group randomised controlled trial (RCT) with 878 participants in the intervention and 1,702 participants in the control group. Setting: The study took place in Hamburg, Germany and made use of health care structures and professionals of a geriatrics centre.
Participants: Study participants were initially community-dwelling, aged 60 years and older and without B-ADL-restrictions, cognitive impairment, or need of nursing care, with sufficient command of the German language.
Interventions: Health promotion and preventive care interventions relied on an extensive health questionnaire and the subsequent offer to participate in multi-topic personal reinforcement performed in small group sessions or at preventive home visits.
Measurements: Primary outcome: Survival time; in some analyses, adjustments were made for gender, age and self-perceived health. Secondary outcome: Functional competence (LUCAS Functional Ability Index) based on responses to self-administered questionnaires at 1-year follow-up and 12 years after 1-year follow-up (2013/2014).
Results: Mean time under observation was 10.3 years. 38.3% (987/2,580) of the participants died; intervention group (IG): 35.7% (313/878), control group (CG): 39.6% (674/1,702); HR=0.89; p=0.09. Functional competence at 1-year follow-up: IG: ROBUST 67.4% (391/580), FRAIL 11.9% (69/580) vs. CG: ROBUST 62.9% (861/1,368), FRAIL 14.8% (203/1,368); p=0.12. 12-years after 1-year follow-up: IG: ROBUST 50.0% (160/320), FRAIL 30.9% (99/320) vs. CG: ROBUST 48.9% (307/628), FRAIL 34.1% (214/628); p=0.56.
Conclusions: Insignificant but consistent effects on survival and the dynamics of functional competence suggest effectivity of the complex intervention. We plan to take a closer look at the effect of each reinforcement separately.
Key words: Healthy ageing, health behaviour intervention, reinforcement strategies, ITT-survival-analysis, functional competence.
Introduction
In view of the steadily increasing life expectancy in developed societies, the WHO recommends health promotion and prevention in old age to assure healthy ageing, to postpone the onset of disability and need of nursing care, and to avoid increasing healthcare expenditures (1-3). Here, we present the long-term results of an RCT done to assess a health promotion and preventive care intervention that had been developed and implemented as part of the PRO-Age study (PRevention in Older people – Assessment in GEneralists’ practices) in Hamburg, Germany between 2001-2002 (4). In 2007, the Hamburg participants of PRO-Age were re-contacted to become participants of the observational Longitudinal Urban Cohort Ageing Study (LUCAS), which is still going on in repeated waves (5, 6). This made possible the evaluation of certain long-term effects of the RCT intervention performed between 2001-2002. Subsequently, in the manuscript, the data base is referred to as “LUCAS study”, implying its beginning as a part of the PRO-Age study.
The one year health promotion and preventive care interventions for initially community-dwelling older persons included a health questionnaire (7, 8) and the offer to participate in reinforcement as organised in small group sessions (9) or by preventive home visits (10). In this RCT, 1-year effects were demonstrated using composite indices of health behaviour and preventive care use. At the 1-year follow-up, the intervention group showed significantly better outcomes than the control group for both these indices. The health behaviour index had an OR of 2.0 (95% CI: 1.6-2.6); the preventive care use index an OR of 1.7 (95% CI 1.4-2.1) (11). No effects were observed regarding the need of nursing care or mortality, as was to be expected because of the short follow-up time (11).
By establishing the LUCAS longitudinal cohort, the follow-up period was extended to over 12 years. Major issues of interest dealt with in the ongoing LUCAS cohort are (5, 6):
(a) To observe and document dynamical aspects of the ageing process in terms of functional competence of older persons. Of central interest are processes of transition, e. g. from the status of robust to frail and disabled. For details, see ref. 5, 12.
(b) To investigate potential long-term effects following the significant favourable effects of the health promotion and preventive care intervention (RCT, 2001-2002) at 1-year follow-up (11) to delineate recommendations how to maintain functional competence.
Here, we present the evaluation of long-term effects of the RCT of health promotion and preventive care done in Hamburg between 2001-2002 in order to analyse sustainability of the positive changes in health behaviour observed in the 1-year follow-up.
Our research questions for this study were:
(1) Does an intention-to-treat analysis (ITT, meaning “analysed as randomised”) of survival show statistically significant differences between the intervention and the control group of the health promotion and preventive care interventions offered between 2001-2002?
(2) Does the long-term development of functional competence, i. e. the combination of an individual’s physical and mental reserves and risks (2), differ between the intervention and the control group in those participants responding to health questionnaires at 1-year follow-up and 12 years after 1-year follow-up (2013/2014)?
Methods
Design of the study
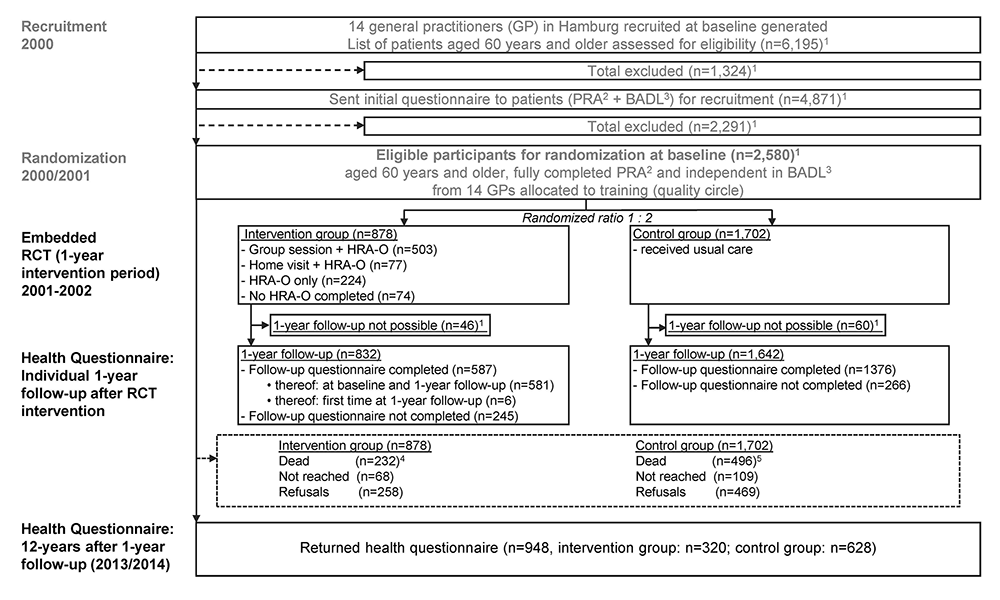
A parallel group randomised controlled trial (RCT) with 878 participants in the intervention and 1,702 in the control group was performed between 2001-2002. Intervention group participants were offered a choice regarding reinforcement according to their individual preferences (Figure 1). Differences in survival were assessed over 13.8 years (165.5 months). Recruitment of participants, data collection and the intervention measures were performed in accordance to the Declaration of Helsinki. Ethical approval was obtained from the Hamburg General Medical Council Ethics Committee and the Data Protection Official of the City of Hamburg (4-6, 11).
Setting
The study took place in Hamburg, Germany’s second largest city with approximately 450,000 persons 60 years or older. The study was coordinated at the Albertinen-Haus, Geriatrics Centre that includes a geriatric hospital department, a day clinic and an outpatient rehabilitation facility, all parts of an academic teaching hospital. The intervention study made use of existing health care structures and professionals and collaborated with an interdisciplinary geriatric team that had been especially trained in health promotion and motivational methods (9).
Participants
Participant recruitment has been described in detail (4, 5, 11) and is illustrated in the flowchart (Figure 1). Briefly, 14 general practitioners with solo practices recruited participants for the RCT over a nine-month period starting in October 2000. Potential participants were identified using complete GP’s patient lists. At baseline (2000/2001), eligible study participants were at least 60 years old, community-dwelling, without restrictions in basic activities of daily living (B-ADL), without need of nursing care (according to the German long-term care legislation), without cognitive impairment and able to understand German. Eligible individuals received the study information letter from their GPs, the PRA questionnaire (Probability for Repeated Admission) measuring six items of baseline risk status for health service use, i. e. person’s age, gender, hospital admissions, visits to GP, health status (heart disease and diabetes status), and caregiver availability (13, 14), one question on B-ADL and the informed consent form. Persons who returned the completed questionnaire and gave written consent were then randomised 1:2 into the intervention and the control group using computer-based randomisation by an external centre (4).
Intervention components
The complex health promotion and preventive care interventions performed in a one year period (2001-2002) have been extensively described (4, 5, 9-11). These interventions included a comprehensive health questionnaire and an offer to participate in personal reinforcement executed in small group sessions or at preventive home visits. All GPs took part in a geriatric quality circle. An overview of the RCT intervention is given in Figure 1.
Notes: 1 For details see: Figure 3 in Stuck et al. BMC Med Res Methodol 2007 and Figure 1 Dapp et al. in J Gerontol A Biol Sci Med Sci 2011. 2 PRA = Probability of Repeated Admissions questionnaire. For details see: Screening elders for risk of hospital admission. Boult et al. in J Am Geriatr Soc 1993. 3 International reference question for need of nursing care (BADL): “Do you need help from someone else with any of the following? a) feeding yourself b) getting to the toilet c) dressing yourself, d) bathing yourself and/or e) moving from bed to chair or standing up?” Answers: “No, I do not need help from someone else” or “Yes, I need help from someone else”. 4 Varying information from Hamburg’s Central Registry (as basis ITT analyses): Dead until reference date 30.09.2014 of the survival analysis (n=313). 5 Varying information from Hamburg’s Central Registry (as basis ITT analyses): Dead until reference date 30.09.2014 of the survival analysis (n=674).
Health questionnaire and computer-generated feedback
After randomisation, the intervention group received the Health Risk Appraisal for Older People (HRA-O). This questionnaire is a validated, multilingual, updated and regionally adapted version for use in older persons in European settings comprising questions on comprehensive health domains i. e. sociodemographic information, self-perceived health, physical activity, nutrition, social network, basic and instrumental activities of daily life and preventative care use. Its development has been described in detail (7, 8, 15). In the intervention group, the information from the questionnaires was used for a computer-generated feedback in text form for each intervention participant who had completed the questionnaire. A summary report was sent to their GPs.
Face-to-face reinforcement
In addition, intervention group participants with filled health risk questionnaires had the choice to participate in one of two different face-to-face reinforcement interventions, either by small group session or by a preventive home visit. The alternative was to reject any reinforcement intervention offered. Thus, intervention group participants were able to choose reinforcement according to their individual possibilities, needs and preferences (4, 11, 16). The concept and issues addressed in these small group sessions and home visits have been described elsewhere (9-11).
In brief, the half-day small group session included a maximum of 12 participants, took place at the geriatric centre, and was led by an interdisciplinary geriatric team trained in health promotion and prevention. At the beginning of each session, a team-leading geriatrician gave comprehensive information on medical aspects of healthy ageing, a physiotherapist informed about physical activity, a nutritionist explained issues of healthy nutrition, and a social worker stressed the importance of active social participation. Together with the health experts, the older persons were then engaged in developing recommendations based on their individual physical activity and dietary records. The participants received individualised written feedback with tailored health-promoting and preventative recommendations (17) within two weeks after the group session to strengthen empowerment and motivation for lasting lifestyle changes. Also, six months after the group session, a follow-up meeting took place at the geriatric centre in order to check adherence to the recommendations (9).
Alternatively, a preventive home visit was conducted by a nurse who was specially trained from the interdisciplinary team at the geriatric centre. At her first visit, the nurse performed a multidimensional assessment to focus on comprehensive health domains. Individual health recommendations were then worked out by the geriatric team. The participant’s GP received a summary report that included both the assessment results and the individual recommendations given to the participant. After six months, a second home visit was made to address and evaluate adherence to health recommendations (10).
Control Group
During the one year intervention period, the participants of the control group received usual care (11).
Outcome variables
In the present analyses, primary outcome was survival time. Survival status was obtained from the Hamburg’s Central Registry, and was double checked using the information from self-administered questionnaires or by GPs’ information. Major efforts have also been undertaken to check mortality status of those participants lost to follow-up or declining study participation at the reference date. If no information was available at the reference day the time on study until the last contact with the study centre or GP was used as time under observation to be used in the survival analysis. The long-term analyses and longest individual survival time amounted to 165.5 months (13.12.2000 – 30.09.2014).
The secondary outcome was functional competence (2, 18) as evaluated by the LUCAS Functional Ability Index (FA Index) (12). The index is based on twelve questions regarding pre-clinical markers of functional competence and includes aspects of physical activity from the health behaviour index used in the 1-year follow-up (12, 19, 20). Furthermore, the FA Index equally includes both marker questions on resources and on risks. Risk marker questions are related to the Fried frailty phenotype (21, 22). The LUCAS FA Index allows categorisation of the functionally heterogeneous group of older persons into four classes of functional ability depending on the presence/absence of resources and risk factors defined as ROBUST (many resources & few risks), postROBUST (many resources & many risks), preFRAIL (few resources & few risks) and FRAIL (few resources & many risks). Our recent survival analyses revealed significant differences between the four LUCAS FA Index classes. The initially ROBUST survived longest, the FRAIL shortest (12).
For the present analyses, the functional classes postROBUST and preFRAIL were taken together as a category termed TRANSIENT (12) in order to assure sufficient numbers and the analyses’ statistical stability.
Information on LUCAS FA Index was obtained at 1-year follow-up and 12 years after 1-year follow-up (2013/2014) in those participants who responded to health questionnaires (5). These health questionnaires integrated key questions from the initial PRA (13, 14) and HRA-O (7, 8, 15) instruments. These questionnaires, incl. the LUCAS FA Index questions, were posed in all waves and supplemented by additional questions on psychological items, physical and mental activities, health literacy, income and use of urban activity space (5). All health related questions used were relevant to independent life and functional status in community-dwelling older people according to a systematic review (23). In addition, the FA Index was validated through comprehensive geriatric assessment instruments (24).
Statistical Methods
In the present study, all study participants of the RCT intervention group received the health questionnaire. All responding members then got the computer-generated feedback report and had the free choice of one of three distinct reinforcements: small group session, preventive home visit or no reinforcement (4, 11). For survival data, analyses included log rank tests and Kaplan-Meier estimators. To increase sensitivity, adjusted analyses were done in addition, using Cox proportional hazard regressions with the covariables gender, age (continuous variable) and self-perceived health (dichotomous: fair/poor vs. other, 25) as a major predictor of mortality (26). All analyses were performed strictly according to the ITT principle, i. e. all participants were analysed as randomised without considering which intervention the participants actually got. No data imputation was made. For the adjusted analyses, we only used the baseline randomisation information (PRA) which was complete by design, and survival information which was also complete.
The analyses of changes in functional competence in both the intervention and the control group were done based on all intervention and control group responders at 1-year follow-up and 12 years after 1-year follow-up (2013/2014). For this secondary endpoint, we worked with the numbers at hand.
T-Tests were used to analyse age, and Pearson’s Chi Square Tests for all other variables. We used STATA 12 (StataCorp 1985-2011) and SPSS 22 (IBM Corp. 1989-2013) and tested with two-sided tests at a 5% level of significance.
Results
Participants’ characteristics
At baseline, there were 2,580 participants in the randomised controlled trial (RCT); intervention group n=878 and control group n=1,702. The intervention and the control group showed comparable participant characteristics, indicating successful randomisation procedure (4, 11). The adjustment variables gender, age and self-perceived health were almost equally distributed. Median age at baseline was 71.1 years (60.3-97.0 y) in the intervention and 70.8 years (60.2-95.8 y) in the control group. Female gender represented 61.5% (540/878) in the intervention and 63.3% (1,077/1,702) in the control group. The proportion of intervention group participants with fair/poor self-perceived health was 38.6% (339/878) and 38.5% (656/1,702) in the control group. Also, results of all further PRA questions (hospital admission, visits to GP, prevalence of chronic diseases, caregiver availability) were similar between intervention and control group (4, 11).
Study participants’ choice of reinforcement
All 878 participants of the RCT intervention group were requested to answer the health questionnaire. Those 804 participants who completed the questionnaire were invited to choose between the reinforcement interventions offered, but not the 74 refusals. 62.5% (503/804) took part in the small group session, 9.6% (77/804) opted for the preventive home visit, and 27.9% (224/804) decided not to choose any reinforcement.
Intention-to-treat analyses on survival
The results of the ITT analyses included all participants who were randomly assigned to the intervention (n=878) and to the control group (n=1,702). The mean time on study was 10.3 years. In total, 38.3% (987/2,580) of the participants died, i. e. 35.7% (313/878) from the intervention group and 39.6% (674/1,702) from the control group (according to Hamburg’s Central Registry). Among these, 41.2% of the participants of the intervention group and 39.6% participants of the control group died while in need of nursing care (data basis: German Health Insurance Medical Service). As displayed in Figure 2, there was almost no difference in the Kaplan-Meier survival curves between intervention and control group until 1,900 observation days (5.2 years). At that point, survival curves separated, and the intervention group showed slightly better survival. However, the difference did not reach statistical significance, log rank test: p=0.09; unadjusted cox regression: hazard ratio (HR)=0.89 (95% CI: 0.78; 1.02). This result was confirmed after adjustment for gender, age and self-perceived health in cox regression: HR=0.89 (95% CI: 0.78; 1.02).
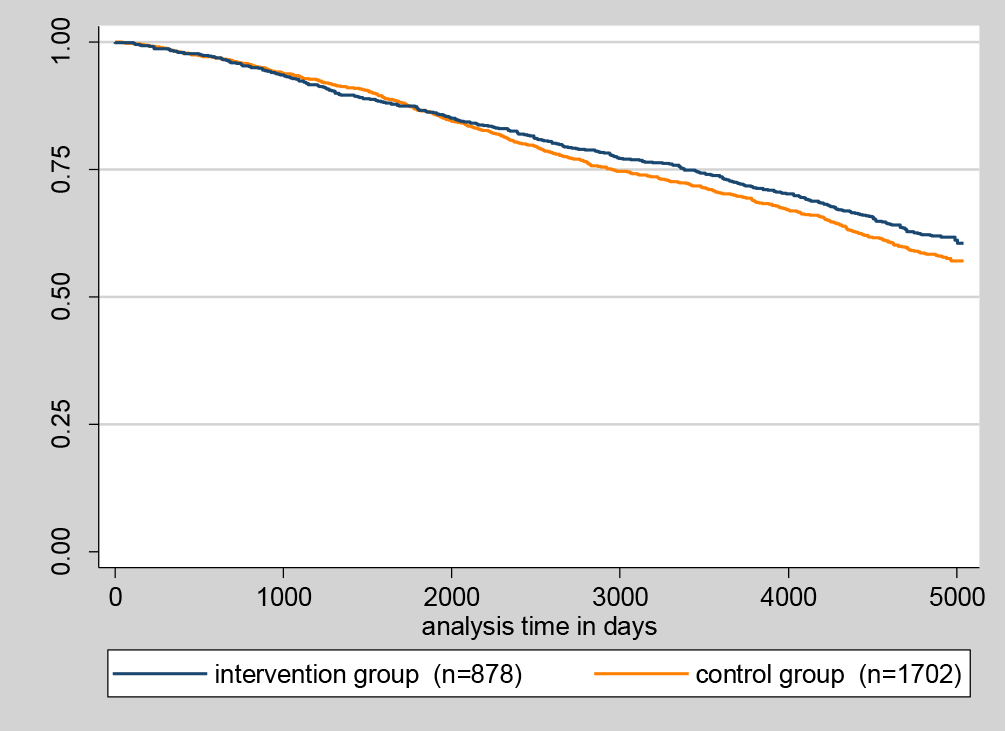
Figure 2: Kaplan-Meier survival curve of the health promotion and preventive care intervention RCT in the long-term perspective of 165.5 months (13.12.2000 – 30.09.2014) based on data from Hamburg’s Central Registry
Development of change in functional competence over time
Responses to the health questionnaires regarding the LUCAS FA Index at 1-year follow-up and 12 years after 1-year follow-up (2013/2014) are given in Table 1. As shown, participation at 1-year follow-up was lower in the intervention group than in the control group. However, in the long-term, the proportions of participation were quite comparable, 36.4% in the intervention and 36.9% in the control group. Also of notice is that median age and proportion of female gender remained almost equal among questionnaire responders in both groups, at both waves. Functional competence according to the LUCAS FA Index showed better results for the intervention group compared to the control group at both analysed waves. However, these differences were not significant (Table 1).
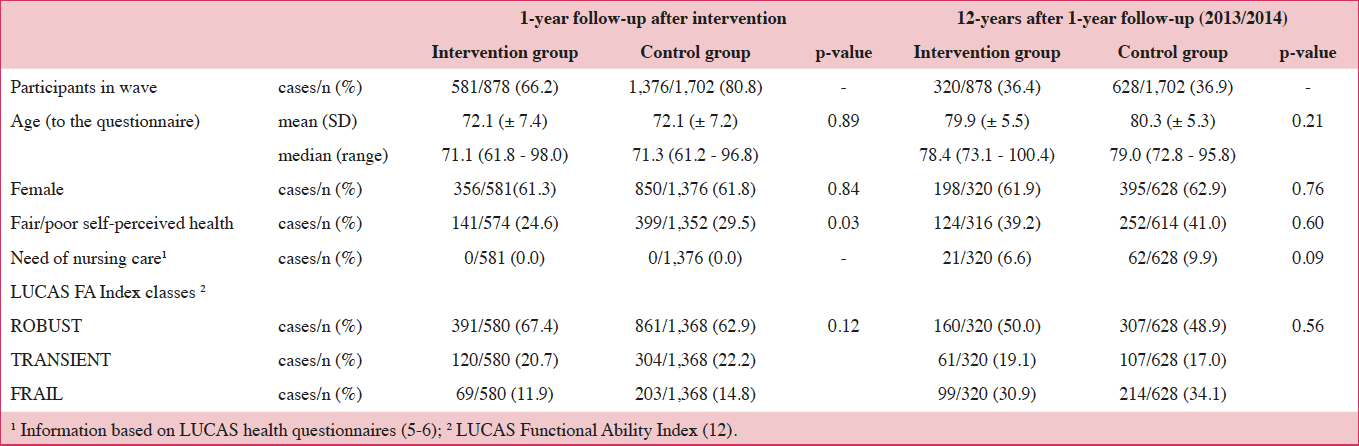
Table 1: Functional competence (LUCAS FA Index) of study participants who responded to health questionnaire at 1-year follow-up and 12 years after 1-year follow-up1
At 1-year follow-up the intervention group participants’ functional competence according to the LUCAS FA Index was: ROBUST 67.4% (391/580), TRANSIENT (postROBUST+preFRAIL) 20.7% (120/580), FRAIL 11.9% (69/580) vs. control group: ROBUST 62.9% (861/1,368), TRANSIENT 22.2% (304/1,368), FRAIL 14.8% (203/1,368); p=0.12. Twelve years after 1-year follow-up intervention-group participants were classified as follows: ROBUST 50.0% (160/320), TRANSIENT 19.1% (61/320), FRAIL 30.9% (99/320) vs. control group: ROBUST 48.9% (307/628), TRANSIENT 17.0% (107/628) and FRAIL 34.1% (214/628); p=0.56 (Table 1).
Over time, there was a shift in functional classes towards FRAIL both in the intervention and the control group. However, even 12 years after 1-year follow-up, almost half of the participants in both groups were categorised as functionally ROBUST. The proportion of participants categorised as TRANSIENT remained at about 20% similar in both groups at both analysed waves, indicating that TRANSIENT is indeed a transitional functional class (Table 1).
Discussion
Summary of major results
We analysed long-term effects of a health promotion and preventive care intervention RCT in community-dwelling people of 60 years and older who had no restrictions in B-ADL and were without need of nursing care at baseline.
The first major finding was that survival over 165.5 months was slightly better in the intervention group compared to the control group, though not statistically significant. The initial coincidence and later divergence of the Kaplan Meier curves may be due to a latent period from behavioural interventions for mortality (27).
Second, changes in the level of functional competence also showed a favourable, however not significant trend in the participants of the intervention compared to the control group.
As a side benefit, we found that even 12 years after 1-year follow-up, roughly half of the responding study participants in the intervention and in the control group were still classified as ROBUST.
The study design allowed intervention group participants to choose between three reinforcements, i. e. not all participants received the same treatment (28-31). Surprisingly, almost two-thirds did choose the small group session (63%), whereas only one tenth chose the preventive home visit (9%). About a quarter decided not to choose (28%) any of the reinforcements offered.
Comparisons with the other PRO-Age trials in London and Solothurn
The London PRO-Age trial, U.K.
In contrast to the Hamburg trial the London trial showed no favourable effects on health behaviours and preventive care use after one year. Long-term comparisons to the London branch of PRO-Age were not possible because the study design of the London trial did not include any follow-up beyond 1-year. Moreover, the study was based on the health risk questionnaire alone, without any interventional reinforcement (32).
The Solothurn PRO-Age trial, Switzerland
Similar to the Hamburg trial that showed favourable effects on health behaviours and preventive care use after one year (11), Stuck et al. presented favourable effects after a 2-year period. In contrast to the Hamburg trial, at Solothurn survival over an 8-year period was significantly better in the intervention than the control group (33).
Findings from the Hamburg RCT and the Solothurn “pragmatic randomised controlled trial” (33) may be different for several reasons.
First of all, study set-ups were quite different: Hamburg had a relatively cheap twice off intervention. The small group sessions and preventive home visits in Hamburg were conceptualised as interventional impulses in order to initiate positive changes in study participants’ health promoting and preventive behaviours. Both small group sessions and preventive home visits took place only twice within the 1-year intervention period (11). Solothurn offered far more extensive and repeated home visits to the intervention group. The Solothurn PRO-Age intervention included repeated home visits by nurses and primary care physician counselling, and was carried out continuously, over a 2 year period (33). Contrary to the Solothurn trial, study participants in Hamburg actively chose small group sessions or preventive home visits or no reinforcement according to their individual preference.
Second, differences between health care systems and cultural background have to be considered. The Hamburg trial took place in an urban population whereas the Solothurn trial participants were rural people. Thus access to and uptake of health services may have been quite different in the two populations (4, 5, 11).
There were also differences in baseline characteristics between the Hamburg and Solothurn PRO-Age trials. Because of the lower age limit of 60 years in Hamburg, the study population was younger than that in Solothurn (age limit 65), and the proportions of females, participants reporting fair/poor health and more frequent GP consultations were higher in the Hamburg compared to the Solothurn trial (4, 11). Another distinct difference was Second World War experiences (displacement, bombing, military recruitment) of the senior citizens in Hamburg (6). Nothing comparable had happened in Switzerland.
Taking the results of the Solothurn and Hamburg trials together, one may tentatively conclude that a preventive health intervention needs to have certain intensity, before it will be of benefit to participants. Such an intervention should best involve both GPs and their patients. The results from an additional study with focus on older persons’ acceptance of preventive home visits provided some evidence to support the rationale of the Hamburg concept of participants’ choice (34). We are not aware of any comparable RCTs on similar complex health behaviour interventions in community dwelling older people. Hence, the level of intensity necessary for success remains unclear, but judging from our (non-significant) effect estimates, group sessions, repeated at two- or three year intervals appear to be serious contenders.
Limitations and Strenghts
A limitation of the present study (and of all long-term intervention studies indeed) is that after the end of the intervention period, both intervention and control group participants could have experienced other interventions on health behaviour and preventive care use. Thus e. g. we know that almost one fifth of the control group participated in a small group session later on.
In addition, both the study participants’ GPs from the intervention and the control group took part in a quality circle (bimonthly training sessions on current topics in geriatric and preventive medicine), that were led by an experienced geriatrician (11). This could have led to a washout of effects.
Another restriction was the lower questionnaire response rate at 1-year follow-up, which can be explained by significantly higher demands on the intervention group (35-page HRA-O questionnaire and small group session or preventive home visit intervention) compared to the control group.
The present study has a number of major strengths. The LUCAS longitudinal cohort is largely representative of the older population in Hamburg (35). Therefore, the health promotion and preventive care interventions presented here reflect well a “real world” setting. E. g. the study population’s characteristics were similar to characteristics of prospective users of such health promotion and preventive care interventional measures. By all indications, selection bias was small because of randomised recruitment. Survival status was double checked using Hamburg’s Central Registry and information from proxy or GPs. Moreover, both base line information and survival response were complete. Utmost care was taken to insure responses were not only complete, but also accurate. The possibility to do adjusted analyses was another strength, insuring that neither bias nor excessive variability jeopardized results.
Considering the fact that the intervention group participants’ were absolutely free to choose between the two forms (small group session or preventive home visit) or to refuse any kind of reinforcement, survival experience and the changes in functional competence may actually have differed between participants with group sessions, with home visits or with no reinforcement – a point we did not investigate here, but which merits future investigation (36).
Conclusions
1. Data collection, checking and organisation of such a long-term study as well as devising and delivering an appropriate intervention was challenging and should not be underestimated.
2. In view of the quite limited intervention, the consistent effects on survival and the dynamics of change in functional competence seen in the intervention group compared to the control group suggest effectiveness of the complex intervention.
3. Although such an intervention seems to maintain or even improve functional ability, it remains an open question whether it will reduce the need for nursing care.
4. Giving participants a choice of intervention according to their inidividual preferences seems to improve participation.
5. There remains a need for further detailed analyses, i. e. investigation of individual transitions over time or subgroup analyses according to the type of reinforcement.
Acknowledgements
We are grateful to all participants involved in this study, to the staff members in the participating GP practices, the president and vice president of the Hamburg Association of General Practitioners, the General Medical Council of Hamburg and the Central Data Protection Act Hamburg, the Central Registry Office Hamburg (Fachamt Einwohnerwesen) and the German Health Insurance Medical Service (Medizinischer Dienst der Krankenversicherung Nord, MDK). We thank Susann Laub, study nurse at the research department of the Albertinen-Haus. She held continuous contact to the more than 3,300 participating senior citizens, and was in charge of data collection. We also thank our data management team Stefan Golgert and Björn Klugmann for preparing statistical analyses, tabulations and graphics. Jennifer Anders MD made major contributions to the LUCAS project earlier on, which are gratefully acknowledged.
Contributions
All authors contributed to the study concept, data interpretation and revisions of the manuscript. In particular: Concept, first draft and final revision of the manuscript: LN, UD, ChEM. Analyses on survival and functional competence: ChEM. WvRK improved the prefinal draft. All authors approved the final version.
Conflict of Interest
All authors report no conflict of interest.
Trial Registration
LUCAS longitudinal cohort study: trial registration number DRKS 00005136 . PRO-Age study: International Standard Randomized Controlled Trial Number: ISRCTN 28458424.
Ethical standard
Ethical approval was obtained from the Hamburg General Medical Council Ethics Committee (Ärztekammer, No. PV-2856) and the Data Protection Official of the City of Hamburg.
Funding
LUCAS (DRKS 00005136) and PRO-Age (ISRCTN 28458424) were supported by grants from the European Union (Brussels, QLK6-CT-1999-02205), the Federal Ministry for Family Affairs, Senior Citizens, Women and Youth (Bundesministerium für Familie, Senioren, Frauen und Jugend; BMFSFJ), the Robert-Bosch Foundation, the Max und Ingeburg Herz Foundation, the Federal Ministry for Education and Research (Bundesministerium für Bildung und Forschung; BMBF LUCAS I: 01ET0708, LUCAS II: 01ET1002A, LUCAS III / PROLONG HEALTH 01EL1407) and the European Commission (LUCAS IV / MINDMAP: HORIZON 2020, research and innovation action 667661). The funding source had no role in the design and conduct of the study, the collection, analyses, and interpretation of the data, the preparation, review, or approval of the manuscript.
References
1. Rechel B, Grundy E, Robine JM, Cylus J, Mackenbach JP, Knai C, McKee M. Ageing in the European Union. Lancet 2013;381:1312-1322.
2. World Health Organisation. World report on ageing and health. Geneva, 2015. http://apps.who.int/iris/bitstream/10665/186463/1/9789240694811_eng.pdf?ua=1. Accessed 20 February 2017.
3. Bousquet J, Kuh D, Bewick M, Standberg T, Farrell J, Pengelly R et al. Operational Definition of Active and Healthy Ageing (AHA): A Conceptual Framework. J Nutr Health Aging 2015;19:955-960.
4. Stuck AE, Kharicha K, Dapp U, Anders J, von Renteln-Kruse W, Meier-Baumgartner HP, Iliffe S, Harari D, Bachmann MD, Egger M, Gillmann G, Beck JC, Swift CG. The PRO-AGE study: an international randomised controlled study of health risk appraisal for older persons based in general practice. BMC Med Res Methodol 2007;7:2.
5. Dapp U, Anders J, von Renteln-Kruse W, Golgert S, Meier-Baumgartner HP, Minder CE. The Longitudinal Urban Cohort Ageing Study (LUCAS): study protocol and participation in the first decade. BMC Geriatr 2012;12:35.
6. Renteln-Kruse von W, Dapp U, Anders J, Pröfener F, Schmidt S, Deneke C, Fertmann R, Hasford J, Minder C. The LUCAS* consortium: objectives of interdisciplinary research on selected aspects of ageing and health care for older people in an urban community. Z Gerontol Geriatr 2011;44:250-255.
7. Stuck AE, Elkuch P, Dapp U, Anders J, Iliffe S, Swift CG; Pro-age pilot study group. Feasibility and yield of a self-administered questionnaire for health risk appraisal in older people in three European countries. Age Ageing 2002;31:463-467.
8. Stuck AE, Kharicha K, Dapp U, Anders J, von Renteln-Kruse W, Meier-Baumgartner HP, Harari D, Swift CG, Ivanova K, Egger M, Gillmann G, Higa J, Beck JC, Iliffe S. Development, feasibility and performance of a health risk appraisal questionnaire for older persons. BMC Med Res Methodol 2007;7:1.
9. Dapp U, Anders J, von Renteln-Kruse W, Meier-Baumgartner H. Active health promotion in old age: methodology of a preventive intervention programme provided by an interdisciplinary health advisory team for independent older people. Journal of Public Health 2005;13:122-127.
10. Renteln-Kruse W von, Anders J, Dapp U, Meier-Baumgartner HP. Preventative home visits by a specially trained nurse for 60-year olds and elderly in Hamburg. Z Gerontol Geriatr 2003;36:378-391 [in German].
11. Dapp U, Anders JA, von Renteln-Kruse W, Minder CE, Meier-Baumgartner HP, Swift CG, Gillmann G, Egger M, Beck JC, Stuck AE; PRO-AGE Study Group. A randomized trial of effects of health risk appraisal combined with group sessions or home visits on preventive behaviors in older adults. J Gerontol A Biol Sci Med Sci 2011;66:591-598.
12. Dapp U, Minder CE, Anders J, Golgert S, von Renteln-Kruse W. Long-term prediction of changes in health status, frailty, nursing care and mortality in community-dwelling senior citizens—results from the Longitudinal Urban Cohort Ageing Study (LUCAS). BMC Geriatr 2014;14:141.
13. Boult C, Dowd B, McCaffrey D, Boult L, Hernandez R, Krulewitch H. Screening elders for risk of hospital admission. J Am Geriatr Soc 1993;41:811-817.
14. Wagner JT, Bachmann LM, Boult C, Harari D, von Renteln-Kruse W, Egger M, Beck JC, Stuck AE. Predicting the risk of hospital admission in older persons–validation of a brief self-administered questionnaire in three European countries. J Am Geriatr Soc 2006;54:1271-1276.
15. Kharicha K, Iliffe S, Harari D, Swift CG, Goodman C, Manthorpe J, Gillmann G, Stuck AE. Feasibility of repeated use of the Health Risk Appraisal for Older people system as a health promotion tool in community-dwelling older people: retrospective cohort study 2001-05. Age Ageing 2012;41:128-131.
16. Kruse A. Gesundheitliche Versorgung. In: Sachverständigenkommission an das Bundesministerium für Familie, Senioren, Frauen und Jugend. Siebter Bericht zur Frage der älteren Generation in der Bundesrepublik Deutschland, Berlin, 2016, pp. 148-180. https://www.siebter-altenbericht.de/. Accessed 20 February 2017.
17. Middleton G, Keegan R, Smith MF, Alkhatib A, Klonizakis M. Brief Report: Implementing a Mediterranean Diet Intervention into a RCT: Lessons Learned from a Non-Mediterranean Based Country. J Nutr Health Aging 2015;19:1019-1022.
18. Bergman H, Beland F, Karunananthan S, Hummel S, Hogan D, Wolfson C: Developing a Working Framework for Understanding Frailty 2004. http://www.frail-fragile.ca/docs/Bergman_2004_English.pdf. Accessed 20 February 2017.
19. Fuchs J, Scheidt-Nave C, Gaertner B, Dapp U, von Renteln-Kruse W, Saum KU, Thorand B, Strobl R, Grill E. Frailty in Germany: status and perspectives: Results from a workshop of the German Society for Epidemiology. Z Gerontol Geriatr 2016;49:734-742 [in German].
20. Renteln-Kruse von W, Minder CE. It is Time to Detect Preclinical Signs of Incipient Frailty. J Am Geriatr Soc 2016;64:2166-2167.
21. Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, Seeman T, Tracy R, Kop WJ, Burke G, McBurnie MA; Cardiovascular Health Study Collaborative Research Group. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 2001;56:M146-156.
22. Fried LP, Ferrucci L, Darer J, Williamson JD, Anderson G. Untangling the concepts of disability, frailty, and comorbidity: implications for improved targeting and care. J Gerontol A Biol Sci Med Sci 2004;59:255-263.
23. Stuck AE, Walthert JM, Nikolaus T, Büla CJ, Hohmann C, Beck JC. Risk factors for functional status decline in community-living elderly people: a systematic literature review. Soc Sci Med 1999;48:445-469.
24. Anders J, Pröfener F, Dapp U, Golgert S, Daubmann A, Wegscheider K, von Renteln-Kruse W, Minder CE. Health and competence: detection and decoding using comprehensive assessments in the Longitudinal Urban Cohort Ageing Study (LUCAS). Z Gerontol Geriatr 2012;45:271-278 [in German].
25. Nishi A, Kawachi I, Shirai K, Hirai H, Jeong S, Kondo K. Sex/Gender and Socioeconomic Differences in the Predictive Ability of Self-Rated Health for Mortality. PLoS ONE 2012;7:e30179.
26. Mossey JM, Shapiro E. Self-rated health: a predictor of mortality among the elderly. Am J Public Health 1982;72:800-808.
27. Hooper L, Bartlett C, Davey Smith G, Ebrahim S. Systematic review of long term effects of advice to reduce dietary salt in adults. BMJ 2002;325:628.
28. Abraha I, Montedori A. Modified intention to treat reporting in randomised controlled trials: systematic review. BMJ 2010;340:c2697.
29. Abraha I, Cherubini A, Cozzolino F, De Florio R, Luchetta ML, Rimland JM, Folletti I, Marchesi M, Germani A, Orso M, Eusebi P, Montedori A. Deviation from intention to treat analysis in randomised trials and treatment effect estimates: meta-epidemiological study. BMJ 2015;350:h2445
30. Moher D, Hopewell S, Schulz KF, Montori V, Gøtzsche PC, Devereaux PJ, Elbourne D, Egger M, Altman DG; CONSORT. CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. Int J Surg 2012;10:28-55.
31. Gupta SK. Intention-to-treat concept: A review. Perspect Clin Res 2011;2:109-112.
32. Harari D, Iliffe S, Kharicha K, Egger M, Gillmann G, von Renteln-Kruse W, Beck J, Swift C, Stuck A. Promotion of health in older people: a randomised controlled trial of health risk appraisal in British general practice. Age Ageing 2008;37:565-571.
33. Stuck AE, Moser A, Morf U, Wirz U, Wyser J, Gillmann G, Born S, Zwahlen M, Iliffe S, Harari D, Swift C, Beck JC, Egger M. Effect of health risk assessment and counselling on health behaviour and survival in older people: a pragmatic randomised trial. PLoS Med 2015;12:e1001889.
34. Pröfener F, Anders J, Dapp U, Minder CE, Golgert S, von Renteln-Kruse W. Acceptance of preventive home visits among frail elderly persons. Participants and non-participants in a follow-up after 2 and 4 years within the LUCAS longitudinal study. Z Gerontol Geriat 2016;49:596-605 [in German].
35. Dapp U, Dirksen-Fischer M, Rieger-Ndakorerwa G, Fertmann R, Stender KP, Golgert S, von Renteln-Kruse W, Minder CE. Comparability of studies of epidemiological research on ageing: Results from the Longitudinal Urban Cohort Ageing Study (LUCAS) and three representative Hamburg cross-sectional studies of healthy aging. Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 2016;59:662-678 [in German].
36. Janevic MR, Janz NK, Dodge JA, Lin X, Pan W, Sinco BR, Clark NM. The role of choice in health education intervention trials: a review and case study. Soc Sci Med 2003;56:1581-1594.