L. Rapp1, S. Sourdet2, B. Vellas2, M.-H. Lacoste-Ferré1,2
1. Faculté de Chirurgie Dentaire, Université Toulouse 3 – Paul Sabatier, Toulouse, France; 2. Pôle Gériatrie, CHU de Toulouse, Gérontopôle, Toulouse, France.
Corresponding author: Dr. Marie-Hélène Lacoste-Ferré, DDS, PhD, Pôle Gériatrie, CHU de Toulouse, Gérontopôle, Toulouse, France , Faculté de Chirurgie Dentaire, Université Toulouse 3 – Paul Sabatier, Toulouse, France, lacoste.mh@chu-toulouse.fr
Care Weekly 2017;1:14
Published online November 9, 2017, http://dx.doi.org/10.14283/cw.2017.5
Please, note that this editorial was published also in the Journal of Frailty Aging (JFA) http://dx.doi.org/10.14283/jfa.2017.9
Abstract
Introduction: The relationships between oral health conditions and frailty have rarely been explored. A systematic review of frailty components and oral health concluded that differences in study population endpoint criteria and study design cannot establish a relationship between frailty and oral health. Objective: This study aims to describe the distribution of the OHAT (Oral Health Assessment Tool) score in a population of frail subjects and to assess associated parameters (age, socio-economic status, living conditions, education level, nutritional habits, cognitive functioning, autonomy). Design: Cross-sectional observational study among patients referred to the Geriatric Frailty Clinic. Measurements: 1314 patients participated in different standardized tests to evaluate their health status, cognitive and affective functioning, adaptation to usual daily activities, nutritional status, and oral health status. Results: The risk of oral health deterioration was higher with the appearance of frailty: the OHAT increased significantly with the Fried Frailty Score (p<0.001). Physical performance and oral health were correlated (p<0.001). The OHAT score and the MNA (Mini Nutritional Assessment) score were significantly correlated: oral status seemed better for malnourished subjects (p<0.001). Dementia significantly increased the risk of an unhealthy oral status (p<0.001). There was no significant correlation between oral status and depression, just a trend. Conclusion: This pilot study establishes a relationship between the OHAT and Fried Frailty Criteria in a population of frail elderly. It must be expanded to follow the distribution of the different items composing the OHAT score (items assessing lips; tongue; gums and tissues; saliva; natural teeth; dentures; oral cleanliness; and dental pain) with different parameters (age, socio-economic status, living conditions, educational level, medical history, drug treatment, nutritional habits, cognitive functioning, disabilities and handicaps).
Key words: Frailty phenotype, physical performance, malnutrition, prevention.
Introduction
After the age of 60 years, because of changes in physical and cognitive health and psychosocial living conditions, the population of elderly adults is heterogeneous, and can be divided into 3 groups: robust older adults, frail older adults, and dependent older adults (1, 3).
Robust older adults age successfully and often have few comorbidities. They have a high level of functioning and can take care of themselves, their health, hygiene and particularly their oral care. They are not different from younger adults in regards to oral care.
Dependence refers to the partial or total inability to perform basic activities of daily life without help. Many studies have shown that the dependent population usually exhibits poor oral health. In the geriatric nursing home, oral health is often neglected, and oral care is considered difficult because of behavior disorders, lack of cooperation, and loss of autonomy, which impair good access to dental health care (4-6).
Frailty is a clinical geriatric syndrome characterized by a decrease in energy reserve, strength and performance, resulting in a progressive decline in multiple physiological systems leading to a state of greater vulnerability. This is defined as a pre-disability state which, different from disability, is still amenable to intervention and is reversible (2-3, 7-8).
The relationship between oral health conditions and frailty has rarely been explored (9). Moreover, it is also necessary to associate general diseases (such as diabetes, rheumatoid arthritis, stroke, or cardiovascular disease), with frailty and oral health. Comorbidities have an undeniable impact on frailty. General health and oral health are interrelated and have a complex and multifaceted relationship, especially in elderly adults.
The elderly have a wide variety of oral health problems, including loss of teeth, edentulism, periodontitis, coronal and root caries, oral mucosal lesions, utilization of nonfunctional dental prostheses, xerostomia and chewing problems, among others (6). Oral health is instrumental to older people’s health, life satisfaction, quality of life, and self-perception (10-11). Oral infections may have biological consequences that later manifest as health problems (12). Oral status can also contribute to changes in diet, weight and physical functioning (13-14). Hence, poor oral health can affect the individual’s overall well-being.
This study aims to describe the distribution of the OHAT (Oral Health Assessment Tool) score in a population of frail subjects, and to assess its correlation with associated parameters (age, socio-economic status, living conditions, education level, nutritional habits, cognitive functioning, autonomy).
Methods
Participants and study design
Cross-sectional observational study of patients referred to the Geriatric Frailty Clinic. The Geriatric Center of Toulouse (i.e., the Gerontopole of the Toulouse University Hospital, in association with the university department of General Medicine and the Midi-Pyrenees Regional Health Authority) designed and developed the innovative “Geriatric Frailty Clinic (GFC) for assessment of frailty and prevention of disability” in 2011. Patients participate in different standardized tests to evaluate their health status, cognitive and affective functioning, adaptation to usual daily activities, nutritional status, and oral health status. All collected data are systematically computerized in a database that can be used for research purposes and statistical analyses. 1314 patients have already been evaluated in the clinic and are included in the study, without any exclusion criteria (15).
Data collected
Tables 1 and 2 recapitulate the data collected and the tests performed in the study.
![Table 2 Oral Evaluation OHAT [0-4 = Healthy, 4-8 = Mild healthy requiring oral attention, 8-12 = Unhealthy, requiring care, 12-16 = Unhealthy, requiring compulsory care]](https://www.vitality-medicine-and-engineering-journal.com/wp-content/uploads/2017/11/FIG-2-LACOSTE.gif)
Table 2
Oral Evaluation OHAT [0-4 = Healthy, 4-8 = Mild healthy requiring oral attention, 8-12 = Unhealthy, requiring care, 12-16 = Unhealthy, requiring compulsory care]
Nutritional evaluation
– Mini Nutritional Assessment (MNA) (16)
The Mini Nutritional Assessment (score /30) is a validated nutrition screening and assessment tool that can identify geriatric patients aged 65 and above who are malnourished or at risk of malnutrition.
– Body Mass Index (BMI) (17)
Body Mass Index (BMI) classifications were developed based on associations between BMI, chronic disease, and mortality risk in healthy populations. The formula of BMI is kg/m2 where kg is the person’s weight in kilograms and m2 is his height in meters squared.
Functional evaluation
– Frailty Status (2)
Five criteria defined by Fried characterize frailty: weight loss, exhaustion, low physical activity, slowness, weakness. The sum score of these five criteria classifies the elderly as not frail (score 0), pre-frail (score 1-2) and frail (score 3-5).
– Activities of Daily Living (ADL) and Instrumental Activities of Daily Living (IADL) (18, 19)
Activities of Daily Living scale is the most appropriate instrument to assess functional status. The ADL ranks adequacy of performance in the six functions of bathing, dressing, toileting, transferring, continence, and feeding. Scores range from 0 to 6, with a score of 1 point if totally independent, 0.5 if partially dependent and 0 if totally dependent in each of the 6 assessed activities.
Instrumental activities of daily living are the activities that people engage in when they are up, dressed and put together. These tasks support an independent life style. Many people can still live independently even though they need help with one or two of these IADLs. They include: cooking, driving, using the telephone or computer, shopping, keeping track of finances and managing medications.
– Short Physical Performance Battery (SPPB) (20)
The Short Physical Performance Battery (Score /12) is a simple test to measure lower extremity function using tasks that mimic daily activities. The SPPB examines 3 areas of lower extremity function: static balance, gait speed, and getting in and out of a chair. These areas represent essential tasks important for independent living.
Cognitive and affective evaluation
– Mini Mental State Examination (MMSE) (21)
The Mini Mental State Examination (Score /30) is a tool that can be used to systematically and thoroughly assess mental status. It is a 30 question test that assesses five areas of cognitive function: orientation, registration, attention and calculation, recall, and language.
– Geriatric Depression Scale (GDS) (22)
The 15 item GDS is a self or hetero-rating scale. Patients are asked to respond based on how they have felt in the last week. The scale uses a yes-no format to be clearer for older patients.
Oral evaluation
– Oral Health Assessment Tool (OHAT) (23, 24)
The Oral Health Assessment Tool (OHAT) provides a global indication of oral health based on observation, conducted whatever the general health of the patient (cognitive state), by a physician, dentist or nurse. It is a recent version of the BOHSE (Brief Oral Health Status Examination), validated by Chalmers et al. in 2005.
The OHAT assesses 8 areas: lips, tongue, gums and tissues, saliva, natural teeth, dentures, oral cleanliness and dental pain. A score of 0 (healthy), 1 (oral changes), or 2 (unhealthy) is given to each of the assessment categories, and a score of the eight categories is summed to give a total oral health score.
Statistical aspects
Data from the 1314 patients already seen at the Geriatric Frailty Clinic were analyzed on SAS® (SAS Institute Inc., Cary, NC, USA) statistical software.
A description of the study sample was first provided, which included: distribution of categorical variables (number and percentage), mean, median, standard deviation, interquartile range, minimal and maximal values of continuous variables.
The global OHAT score was analyzed as a continuous variable. Each of its components was analyzed as a categorical variable (including three categories: 0, 1, 2).
The usual tests were used to assess univariate associations between OHAT scores and other clinical variables (age, socio-economic status, living conditions, education level, medical history, drug treatments, nutritional habits, cognitive functioning, disabilities and handicaps). The Chi square test (or Fisher’s exact test when conditions required for the Chi square test were not fulfilled) was used to compare categorical variables. Student’s t-test (or the Kruskal Wallis test) was used to compare the distribution of a continuous variable between categories of a categorical variable. Pearson’s (or Spearman’s) correlation coefficient was estimated to assess the strength of the link between continuous variables.
Ethical considerations
The study protocol was approved by the local Research Ethics Committee (Comité d’Ethique de la Recherche des Hôpitaux de Toulouse). It did not require either a verbal or a written consent from participants, as this study collected and analyzed only data and information from usual care during hospitalization (without any further assessment, experimentation, procedures, or follow-up). Patient records and information were anonymized and de-identified prior to analysis.
Results
Patient Characteristics (Tables 1-2)
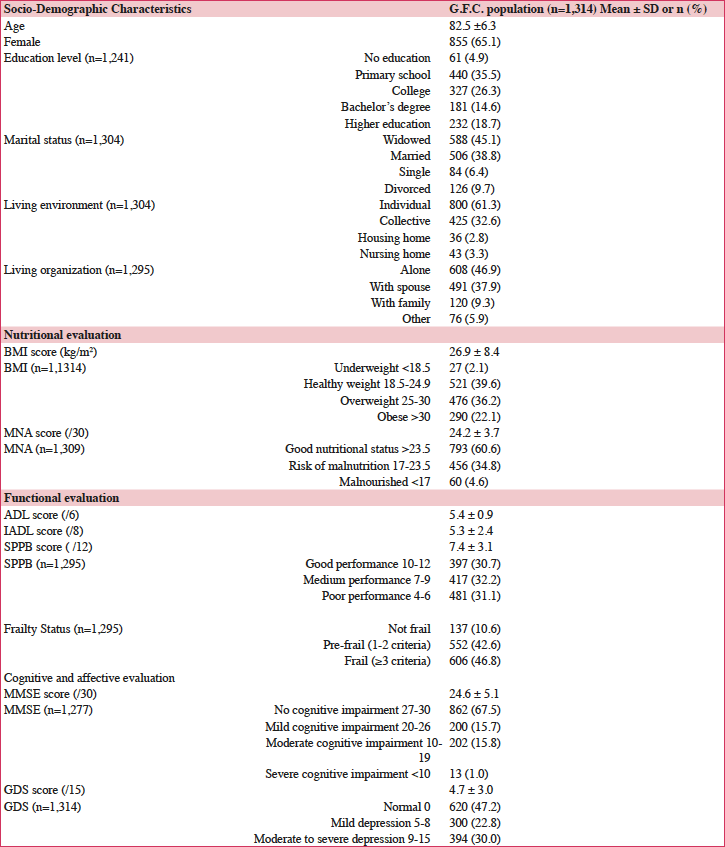
The description of the main characteristics of the 1314 patients recruited is reported in Tables 2, 3 and 4. Participants had a median age of 82.5 (SD 6.3), range 76.2-88.8 years. Most patients were women (65.1%). Most participants (n=1254, 95.1%) had gone to school, but few of those had attended higher education (n=232, 18.5%). Most participants were widowed (45.1%), single (6.4%) or divorced (9.7%). The living environment was individual (61.3%). There were 46.9% participants living alone at home.
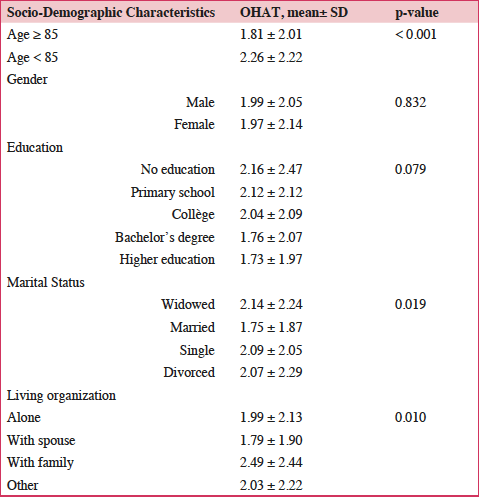
Table 3
Bivariate analysis of OHAT according to socio-demographic characteristics (OHAT = continuous variable)
According to the Fried definition of frailty, 552 subjects were pre-frail (42.6%) and 606 subjects were frail (46.8%).
Concerning the functional evaluation, physical performances were good for 397 subjects (30.7%). Concerning autonomy, the mean ADL score was 5.4 ±0.9 and the mean IADL score was 5.3 ±2.4.
For the BMI, the mean score was 26.9 ±8.4 and only 27 participants were underweight (2.1%). Regarding the nutritional evaluation, 793 (60.6%) participants presented a good nutritional status, 456 (36.8%) participants presented a risk of malnutrition and 60 (4.6%) participants were malnourished. Concerning the cognitive evaluation, the mean MMSE score was 24.6 ±5.1. Moderate to severe dementia was observed in 215 (16.8%) participants, with a MMSE score < 19. For the affective evaluation, the mean GDS score was 4.7 ±3.0. Moderate to severe depression was detected in 394 subjects (30%). Concerning the oral evaluation, the mean OHAT score was 1.98 ±2.1. Most subjects (n=1029, 79.7%) had an OHAT score < 4; they presented good oral health.
Relationships between oral health and socio-demographic characteristics (Table 3)
Statistical analysis showed no significant difference between women and men or according to education level. The OHAT decreased with age (p<0.001). The difference was significant according to marital status and living conditions; participants who were married and participants who lived with their spouse had better oral health.
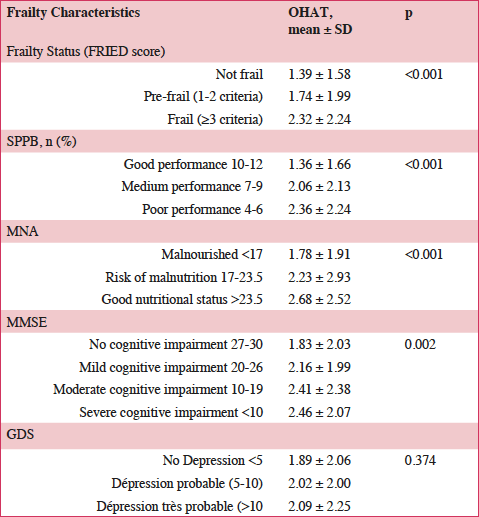
Relationships between oral health and the functional, nutritional, cognitive and affective evaluation (Table 4)
The risk of oral health deterioration was higher with the appearance of frailty: the OHAT increased significantly with Fried Frailty Score (p<0.001). Physical performance and oral health were correlated (p<0.001). The OHAT score and the MNA score were significantly correlated: oral status seemed better for malnourished subjects (p<0.001). Dementia significantly increased the risk of unhealthy oral status (p<0.001). There was no significant correlation between oral status and depression, just a trend.
Discussion
Published studies on the relationship between oral health and frailty have not provided strong conclusions because oral health and frailty criteria measurements and the study designs were different (9). Target populations were not homogenous. Only 75% of the participants in a Mexican study had an oral examination (25). In a Japanese study, the distribution of frail, pre-frail and robust people did not agree with the current distribution (26). Most studies used handgrip strength as the frailty criteria (9). Concerning the oral examination, there is no possible comparison because of variations in criteria such as the number of teeth or number of functional teeth, comfort or pain, use of prosthesis or need for prosthesis, periodontal pocket or periodontitis (25-28). Moriya et al. used a validated index: the General Oral Health Assessment Index (GOHAI) combined with handgrip strength (29). But the GOHAI is a self-questionnaire, only usable by patients without cognitive impairment.
Our pilot study provides a complete screening of frailty and a global oral examination for persons aged 65 years and older considered frail by their physician. Frailty criteria are based on international validated scales (2). The oral health evaluation is based on the OHAT, which is a global oral health index conducted by a GFC geriatrician or nurse. The OHAT can be carried out whatever the cognitive, psychic, or physical health condition of the patient. It involves locating damage affecting the whole mouth. It is not a diagnostic tool, because it does not specify the number of teeth or the severity of the pathologies (caries, severe periodontitis). It does not assess oral function (number of functional units, chewing ability). Furthermore, the OHAT orients care needs by identifying degraded areas (23-24). It can explain the unexpected results with age and nutritional status. In fact, an edentulous patient without prosthesis can constitute a bias; he presents no dental or gingival diseases because he has no teeth, daily oral hygiene is easier, and only the item “prosthesis” can be scored as 2. However, because he is edentulous, he cannot chew correctly and consequently will select food. Thus, the OHAT score for an edentulous patient without prosthesis can be lower than that of dentate patients with 4 or 5 caries and gingival disease because of poor oral hygiene. A mouth with dental or periodontal disease may maintain acceptable function but will remain damaged. Also, the oldest patients are frequently edentulous, without complete dentures. Watanabe et al. described the associations between frailty, age and oral function (number of functional teeth, number of teeth present, occlusal force, masseter muscle thickness, and oral diadochokinesis) (26).Even when they had as many functional teeth as the pre-frail and the robust, the frail oldest had a decrease of occlusal force, and their performance was decreased in the phonetic test (oral diadochokinesis).
Although the MNA is commonly used by geriatricians, weight loss indicates nutritional status for most of the studies concerned with oral health and frailty. However, their conclusions are contradictory. Weight loss and oral health are still not correlated, particularly the edentulous and loss of teeth categories. Patients with poor oral health have difficulty in maintaining an appropriate diet; they adapt and select foods, and they eat more sweet foods, which do not result in weight loss (9).
The results of this pilot study show that oral health deteriorates significantly with the advance of frailty. It is prefigured in many studies: very poor oral health is observed with dependence, because of the low perception of oral health, neglected dental check-up visits and poor daily oral hygiene (6). Access to dental care is often decried for elderly people. Cost, availability and accessibility constitute commonly recognized barriers to the use of dental services (5, 11). The decrease in physical performance could also be another barrier to dental care. Castrejon-Perez et al. underline the fact that the low utilization of dental services could be considered a possible risk marker for frailty syndrome (25). The oral health of patients living with a spouse is better than that of patients living alone; accompaniment to the dental office can be facilitated. The worst OHAT score was among patients who live with family; it seems that family reunification does not help to support satisfactory oral health, because of the break with dental maintenance.
Oral health deteriorates with progressive cognitive disease. Patients with severe cognitive impairment have the worst oral disease. Many studies have described the same results (30). It is necessary to insist on the importance of dental maintenance from the first signs of dementia. Patients with Alzheimer’s disease progressively lose the ability to care for themselves. This is true for oral care, especially for dental and prosthetic hygiene.
Conclusion
In conclusion, general health and oral health are interrelated and have a complex and multifactorial relationship, especially in frail elderly people. This pilot study demonstrates the relationship between the OHAT and the Fried Frailty Criteria in a population of frail elderly. It should be expanded to follow the distribution of the different items composing the OHAT score (items assessing lips; tongue; gums and tissues; saliva; natural teeth; dentures; oral cleanliness; and dental pain) with different parameters (age, socio-economic status, living conditions, education level, medical history, drug treatment, nutritional habits, cognitive functioning, disabilities and handicaps). Thus, it will allow the following possibilities:
– Identification of oral health as a possible criterion of frailty
– Screening of the frail population at the first sign of oral degradation and development of monitoring adapted to this targeted population
– Education of the elderly on geriatric oral health principles: oral hygiene, curative care
Conflict of Interest
None reported by authors.
References
1. Sourdet S, Rouge-Bugat ME, Vellas B, Forette F. Frailty and aging. J Nutr Health Aging 2012;16:283-4.
2. Fried LP, Tangen CM, Walston J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 2001;56:M146–56.
3. Clegg A, Young J, Iliffe S, Rikkert MO, Rockwood K. Frailty in elderly people. Lancet 2013;381:752–62.
4. Boczko F, McKeon S, Sturkie D. Long-Term Care and Oral Health Knowledge. J Am Med Dir Assoc 2009;10:204–6
5. Jablonski RA, Lunro CL, Grap MJ, Elswick RK. The role of behavioral, environmental, and social forces on oral health disparities in frail and functionally dependent nursing home elders. Biol Res Nursing 2005;7:75-82.
6. Thomson WM. Epidemiology of oral health conditions in older people. Gerodontology 2014;31:9-16.
7. Fulop T, Larbi A, Witkowski JM, McElhaney J, Loeb M, Mitnitski A, Pawelec G. Aging, frailty and age-related diseases. Biogerontology 2010;11:547-63.
8. De Carvalho Mello A, Montenegro Engstrom E, Correia Alves L. Health-related and socio-demographic factors associated with frailty in the elderly: a systematic literature review. Cad.Saude Publica 2014;30:1143-68.
9. Nascimento Torres LH, Tellez M,Balbinot Hilgert J, Neves Hugo F, Rosario de Sousa ML, Ismail AI. Frailty, frailty components, and oral health: a systematic review. J Am Geriatr Soc; 2015;63:2555-62.
10. Miura H, Yamasaki K, Morizaki N, Moriya S, Sumi Y. Factors influencing oral health-related quality of life (OHRQoL) among the frail elderly residing in the community with their family. Arch Gerontol Geriatr 2010;51:62-5.
11. Niesten D, Van Mourik K, Van Der Danden W. The impact of having natural teeth on the QoL of frail dentulous older people. A qualitative study. BMC Public Health 2012;12:839.
12. Kuo LC, Polson AM, Kang T. Associations between periodontal diseases and systemic diseases: A review of the inter-relationships and interactions with diabetes, respiratory diseases, cardiovascular diseases and osteoporosis. Public Health 2008;122:417–33.
13. Walls AWG, Steele JG. The relationship between oral health and nutrition in older people. Mech Ageing Dev 2004;125:853-7.
14. Sumi Y, Ozawa N, Miura H, Michiwaki Y, Umemura O. Oral care help to maintain nutritional status in frail older people. Arch Gerontol Geriatr 2010;51:125-8.
15. Tavassoli N, Vellas B et al. Description of 1,108 older patients referred by their physician to the “Geriatric Frailty Clinic (GfC) for assessment of frailty and prevention of disability” at the gerontopole. J Nutr Health Aging 2014;18:457-64.
16. Guigoz Y, Vellas B. The Mini Nutritional Assessment (MNA) for grading the nutritional state of elderly patients: presentation of the MNA, history and validation. Nestle Nutr Workshop Ser Clin Perform Programme 1999;1:3-11; discussion 11-12.
17. Ford DW, Jensen GL, Still C, et al. The associations between diet quality, body mass index (BMI) and health and activity limitation index (HALEX) in the Geisinger rural aging study (GRAS). J Nutr Health Aging 2014;18:167–70.
18. Katz S, Ford AB, Moskovitz RW, Jackson BA, Jaffe MW. Studies of illness in the aged. The index of ADL: a standardized measure of biological and psychosocial function. JAMA 1963;185:914-9.
19. Katz S. Assessing self-maintenance: Activities of daily living, mobility and instrumental activities of daily living. J Am Getriatr Soc 1983;31:721-6.
20. Guralnik JM, Simonsick EM, Ferrucci L, et al. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol 1994;49:M85-94.
21. Folstein M, Folstein SE, McHugh PR. “Mini-Mental State” a Practical Method for Grading the Cognitive State of Patients for the Clinician. J Psych Res 1975;12;189-98.
22. Sheikh JI, Yesavage JA. Geriatric depression scale: recent evidence and development of a shorter version. Clin Gerontol 1986;5:165-72.
23. Chalmers JM, King PL, Spencer AJ, Wright FAC, Carter KD. The oral health assessment tool – validity and reliability. Austra Dental J 2005;50:191-9.
24. Chalmers JM, Pearson A. A systematic review of oral health assessment by nurses and carers for residents with dementia in residencial care facilities. Special Care Dentist 2005;25:227-33.
25. Castrejon-Perez RC, Borges-Yaneez SA, Gutierrez-Robledo LM, Avila-Funes JA. Oral health conditions and frailty in Mexican community-dwelling elderly: a cross sectional analysis. BMC Public Health 2012;12:773.
26. Watanabe Y, Hirano H, Arai H, et al. Relationship between frailty and oral function in community-dwelling elderly adults. J Am Geriatr Soc 2016 (in press)
27. Niesten D, Van Mourik K, Van Der Sanden W. The impact of frailty on oral care behavior of older people: a qualitative study. BMC Oral Health 2013;13:61.
28. De Andrade FB, Lebrao ML, Santos JL, Duarte YA. Relationship between oral health and frailty in community-dwelling elderly individuals in Brazil. J Am Geriatr Soc 2013;61:809-814
29. Moriya S, Tei K, Murata A et al. Relationships between Geriatric Oral Health Assessment Index scores and general physical status in community-dwelling older adults. Gerodontology 2012;29:998-1004.
30. Rodrigues Ribeiro G, Riani Costa JL, Bovi Ambrosano GM, Rodrigues Garcia RCM. Oral health of the elderly with Alzheimer’s disease. Oral Surg Oral Med Oral Pathol Oral Radiol 2012;114:338-43.