Zhaohui Cui1, June Stevens1,2, Jianwen Cai3
1. Department of Nutrition, Gillings School of Global Public Health and School of Medicine, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA; 2. Department of Epidemiology, Gillings School of Global Public Health and School of Medicine, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA; 3. Department of Biostatistics, Gillings School of Global Public Health, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA.
Corresponding to: Zhaohui Cui, 2212 McGavran-Greenberg Hall, Department of Nutrition, Gillings School of Global Public Health, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA 27599. Email: cuizhaohui2008@gmail.com
Care Weekly 2019;
Published online March 11, 2019, http://dx.doi.org/10.14283/cw.2019.2
Abstract
Background: Intentional weight loss has been shown to have health benefits, whereas, unintentional weight loss is a strong risk factor for morbidity and mortality. The prevalence of unintentional weight loss in an American national sample has not been described in the past quarter century.
Objectives: To describe the distribution of unintentional and intentional weight loss and its associations with demographics, smoking, and weight status.
Design: A nationally representative population-based cross-sectional study.
Setting: The National Health and Nutrition Examination Survey (NHANES 1999-2016).
Participants: 41,603 adults who aged ≥21 years and were not pregnant during the year prior to the survey.
Measurements: Participants reported their current body weight, their weight one year earlier, and if they tried to lose weight in the past year. A weight loss was defined as a ≥5% of reduction in weight. Demographics, smoking, and weight status were determined for the beginning of the weight change interval. We used survey frequency analysis to examine prevalences and survey multinomial logistic regression analysis to compare odds ratios in subgroups.
Results: Over a one year period, 18.2% of American adults lost weight, and 6.2% lost weight unintentionally. The prevalence of unintentional weight loss was stable over the 18-year period studied. Adults who were older were more likely to subsequently lose weight unintentionally than their younger counterparts, and the highest risk was in those who were 79 years or older. Other risk factors included lower education level (vs. college educated) and smoking (vs. nonsmoking). Adults who were overweight or obese were more likely to report unintentional weight loss than normal weight.
Conclusion: Studies examining weight loss need to assess and carefully consider the distribution and correlates of intentionality, and expect that even elderly cohorts will exhibit both unintentional and intentional weight loss.
Key words: Unintentional weight loss, intentional weight loss, prevalence, correlates, trends.
Introduction
Unintentional weight loss (UWL) is thought to be a consequence of diagnosed and undiagnosed disease and to be more common in older adults (1, 2). UWL has been less well studied than intentional weight loss (IWL), in part, because UWL cannot be randomized for clinical study. Recent systematic reviews of randomized controlled trials found that IWL improved cardiovascular disease (CVD) risk factors (3) and reduced the risk of all-cause mortality by 15% (4). In contrast, a systematic review of cohort studies found that UWL was associated with a 22% increase in all-cause mortality in adults with overweight or obesity (5). Despite its severe health consequences, population statistics on UWL are very limited and prevalence estimates for the United States are not available for periods after 1989 (1, 2). Since then, some risk factors of UWL have changed (6, 7), and it is likely the population distributions of UWL shown in earlier studies (1, 2) have also changed.
The purpose of this paper is to describe the prevalence of UWL and examine its associations with demographics, smoking, and weight status in adults using data from 1999-2016 National Health and Nutrition Examination Survey (NHANES). Different from the earlier work, where possible, we establish temporal sequence such that the exposures examined were present prior to the time interval of weight loss, and we emphasize associations with age. To provide context we show parallel results on IWL.
Methods
Study Design
The 1999-2016 NHANES investigated a nationally representative sample of the U.S. civilian, noninstitutionalized population assembled using a stratified, multistage probability sampling (8). Selected minority race/ethnic groups, low-income persons, and the elderly people (aged ≥70 years from 1999-2006 and ≥80 years from 2007-2016) were oversampled to provide more reliable estimates for those subgroups. The study protocol was approved by the institutional review board at the Centers for Disease Control and Prevention (Atlanta, GA), and written informed consent was obtained from all participants.
Weight Loss and Intentionality
A trained technician measured height and weight following standard procedures. Participants also reported their current body weight and their weight 1 year earlier. If the differences between the two self-reports indicated a weight loss of ≥10 pounds, participants were asked “was the change between your current weight and your weight a year ago intentional?” All other participants were asked “during the past 12 months, have you tried to lose weight?”
Percent weight change was calculated using the two self-reports. Weight loss was defined as ≥5% of reduction in weight because that amount has been found clinically relevant (9) and is larger than usual day-to-day fluctuation (10). Weight loss was called unintentional if the participant answered “no” to either the question on intentionality or the question on try to lose weight. Body mass index (BMI) at 1 year prior to the survey was calculated using the self-reported weight at that time and measured height.
Correlates
We estimated the level of exposure variables 1 year prior to the clinic examination (at the beginning of the weight change interval). We subtracted one year from assessed age, and individuals who were ≥21 years of age at the time of the examination are called “adults” here. We assumed that the reported sex, race/ethnicity, and education category represented status one year prior to the examination. Participants reported smoking at least 100 cigarettes in their lifetime, current smoking status, the age they started smoking, and the time elapsed since they quit smoking. These variables were used to determine smoking status at 1 year prior to the survey (current smokers, or current non-smokers).
Analytic Sample
We restricted this study to adult participants who were not pregnant during the 1 year prior to the survey. Those missing self-reported weight, height, or intentionality of weight loss (n = 1726), education level (n = 51), or smoking status (n = 224) were excluded from the analysis. Our final analytic sample included 41,603 participants.
Statistical Analysis
All analyses were conducted using SAS (version 9.4; SAS Institute, Cary, NC) and accounted for the complex sample design. We calculated the prevalence of UWL and IWL using survey frequency analysis. Time trends in the prevalence of UWL was studied by plotting 6-year means. Survey multinomial logistic regression analyses were applied to examine the associations of demographics, smoking, and weight status with UWL and IWL (relative to no weight loss). Interactions of sex with age, race/ethnicity, education, smoking status, and weight status were tested. We also conducted a sensitivity analysis to determine the impact of deleting from the analytic sample adults with the largest discrepancies in measured and self-reported current weight.
Results
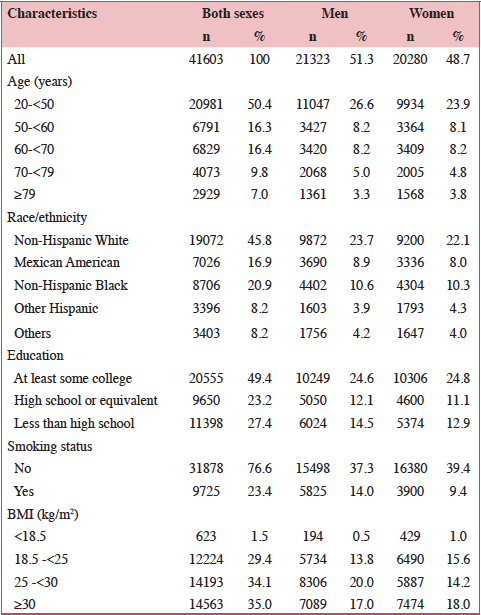
Table 1 describes the study sample and shows that those who were 20-<50 years old, non-Hispanic White, and received at least some college education accounted for approximately half of the sample within the corresponding age, ethnic, and education subgroups. Compared to men, the sample of women included lower proportions of smokers, and overweight individuals. The distributions by age, race/ethnicity, and education were similar between men and women.
The overall prevalence of reported weight loss in the previous year was 18.2%. Table 2 presents population prevalences of UWL and IWL without adjustments for covariates. The prevalence of UWL was 6.2% overall and examination of 6-year means between 1999 and 2016 (data not shown) indicated that the prevalence of UWL was stable over time. The prevalences of UWL and IWL were higher in women than men. Obese men and women had a markedly higher prevalence of IWL as well as a higher prevalence of UWL compared to adults of other weight status. UWL was approximately twice as prevalent in men and women over 79 years of age compared to those younger than 70 years. Figure 1 indicates that the unadjusted prevalence of UWL started to increase at approximately 70 years of age in men and at a younger age in women (approximately 50 years of age). The prevalence of IWL was relatively stable in men while it started to decline at 50 years of age in women.
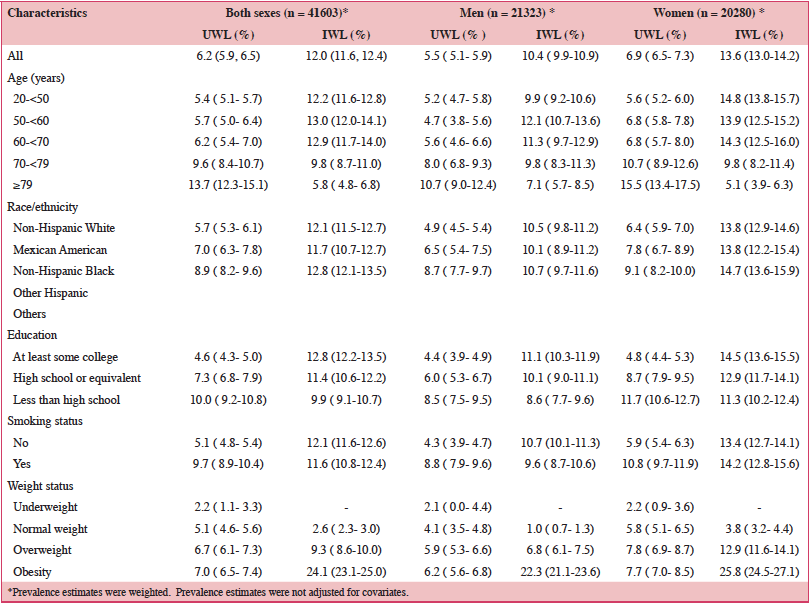
Table 2. Prevalence (95% confidence interval) of unintentional and intentional weight loss overall and by sex
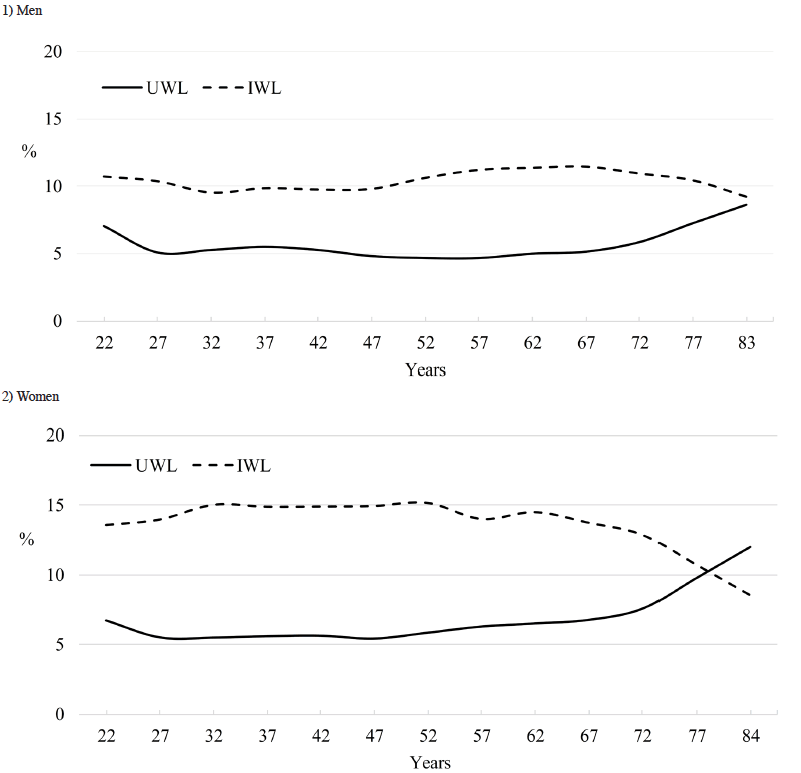
Figure 1. Sex-specific prevalence of unintentional and intentional weight loss in adults*: NHANES 1999-2016
* Prevalence was calculated by 5-year interval in age and smoothed. Age on x-axis is the median of each interval
In Table 3, both UWL and IWL showed significant 2-way interactions of sex with race/ethnicity (p <0.04), but not with smoking (p >0.8). In sex stratified analyses, adults who were ≥79 years of age had approximately 3 times the odds of having UWL compared to those aged 20 to <50 years. The age pattern of IWL was highly discrepant with that of UWL, with the odds ratio not changing over age categories in men, and declining with age in women. Mexican Americans or non-Hispanic Blacks (vs. non-Hispanic Whites), less educated (vs. more educated), and smokers (vs. non-smokers) were more likely to lose weight unintentionally (vs. no weight loss) in the next year. The odds of UWL and IWL were higher in overweight and obese men and women compared to the normal weight and the underweight.
In a sensitivity analysis we examined the impact of errors in self-reported weight. We deleted participants with the 3% and then 5% highest and lowest differences between the current self-reported and measured weights. We found that this maneuver made essentially no difference in the results shown here.
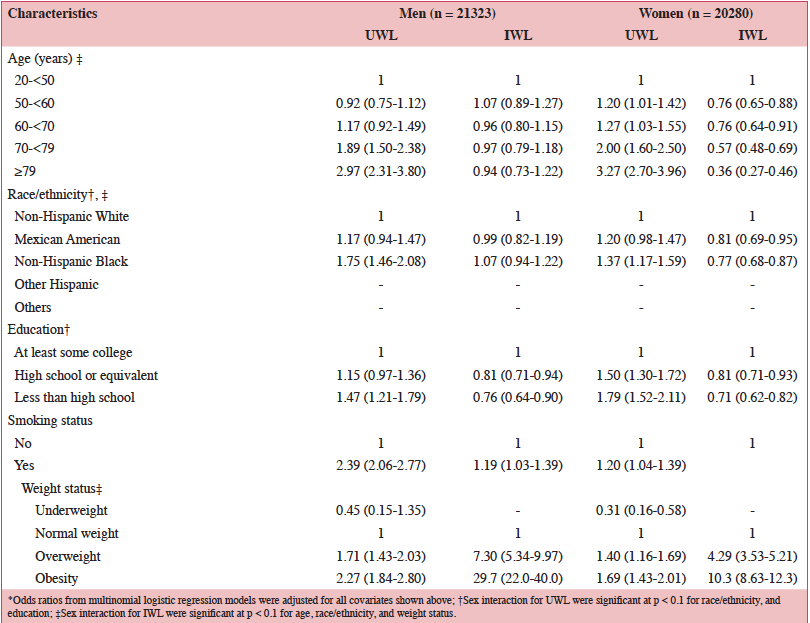
Table 3. Adjusted * odds ratios (95% confidence interval) of unintentional and intentional weight loss relative to no weight loss for demographics, smoking, and weight status by sex
Discussion
Our analyses of recently collected nationally representative data found that approximately 1/3 of the 18.2% of US adults who had lost weight over a year did so unintentionally. Higher likelihood of subsequent UWL were seen in those who were older (vs. younger), Mexican American and non-Hispanic Black (vs. non-Hispanic White), less educated (vs. college educated), and smokers (vs. non-smokers). In addition, UWL was more likely in adults who were overweight or obese compared to normal weight. Although sex interactions were found for race/ethnicity, the directions of associations were consistent in men and women.
We know of two other studies that examined prevalence of UWL using nationally representative data (1, 2). The two studies used data collected in 1980s or earlier and limited their analyses to participants aged ≥45 years. Sahyoun et al. (2) found 6.9% UWL over 6 months in adults aged 50-74 years in NHANES II (1976-1980). Although not shown explicitly, a UWL (over one year) prevalence of approximately 5% can be estimated from data presented by Meltzer and Everhart (1) in adults aged ≥45 years in 1989. These estimates were similar to our estimate of 6.8% in adults with the same age in our study. To our knowledge we are the first to present US national estimates of UWL in adults younger than 45 years, and our plots indicated that the prevalence of UWL in this age group was as high as 5.4%.
Our subgroup analyses by age groups and smoking status generally agreed with the results from these 2 earlier national studies (1, 2), however, there were some discrepancies related to sex, race/ethnicity, education, and weight status that followed no clear pattern. These differences might have been caused by dissimilarities in study methods including length of the time interval of UWL, age ranges of participants, model covariates, and analytic approaches. Also, the order and phrasing of the questions used to establish intentionality were different. These differences in methodology make it difficult to use the 3 national studies to make conclusions concerning the prevalence and attributes of UWL over time. We have greater confidence in our examination of the NHANES data collected from 1999-2016 that showed very little change in the UWL prevalence over 18 years. Over those years consistent methods were used to obtain body weights and intentionality of weight loss.
Our findings, and the results from Sahyoun et al. (2) and Meltzer and Everhart (1) are consistent with those of Wannametthee et al. (11) who found that adults with UWL were more likely to be older compared to those who did not report UWL after adjusting for covariates. In our overall analysis the prevalence of UWL was more than doubled in adults ≥ 79 years of age (13.7%, 95% CI: 12.3%, 15.1%) compared to those 20 to <50 years (5.4%, 95% CI: 5.1%, 5.7%). Nevertheless, it is noteworthy that although most weight loss was unintentional in older age groups, IWL was found in 7.1% of men and 5.1% of women over 79 years of age. Even in this older group, it should not be assumed that all weight loss is disease-induced or unintentional. Similarly, in all the subgroups studied, with the one exception of adults who were underweight, both intentional and unintentional weight loss were observed in a non-trivial proportion of the American population that was statistically significant (i.e., confidence interval did not included zero). Given the contradictory health outcomes associated with the intentionality of weight loss, observational studies of total weight loss, with no indication of intentionality, should be interpreted with caution.
It is a concern that the intentionality of weight change cannot be objectively assessed and is only feasible to know from self-report. It is possible that an unintentional weight change could be mistakenly attributed to a change in behavior or a perceived change in behavior and called intentional. Although we cannot objectively measure intentionality, we can know perceived intentionality. Albeit imperfect, we believe that participant report of intentionality is the best assessment currently available in observational studies.
It is a weakness of this work that weight change was determined using participant-reported body weight. Many cross-sectional studies have evaluated accuracy of self-reported weight in adults and found high correlations of approximately 0.9 between the two measures, even though there is bias across weight status groups (12, 13). Since participants tend to underreport their weight, and this exaggeration may be greater in reports of past weight (14), the prevalence of UWL in our study may be conservative. Our sensitivity analysis provided some level of confidence that errors in self-reported current weight did not unduly influence our results. Unfortunately, we had no objective measures with which to compare the self-reported weight one year prior to the examination. Two measured weight measurements over the 1 year period would have produced more valid measures of weight change.
We consider use of nationally representative data, and the large sample sizes produced by combining data collected over 18 years strengths. Also, we used a study design that sought to establish temporal sequence. Our study is the first to report the prevalence of UWL in adults younger than 45 years and one of very few to focus on UWL. IWL has been far better studied than UWL, and since 2005 several investigators have used recent NHANES data to study issues related to IWL (15, 16, 17, 18). Our side-by-side examinations of UWL and IWL provide a greater understanding of the role of intentionality of weight loss. Future studies need to provide more information on possible causes of UWL as well as more insights into its consequences.
Disclosure
The authors declared no conflict of interest. Dr. Cui has nothing to disclose. Dr. Stevens has nothing to disclose. Dr. Cai has nothing to disclose.
References
1. Meltzer AA, Everhart JE. Unintentional weight loss in the United States. Am J Epidemiol 1995;142: 1039-1046.
2. Sahyoun NR, Serdula MK, Galuska DA, Zhang XL, Pamuk ER. The epidemiology of recent involuntary weight loss in the United States population. J Nutr Health Aging 2004;8: 510-517.
3. Zomer E, Gurusamy K, Leach R, Trimmer C, Lobstein T, Morris S, et al. Interventions that cause weight loss and the impact on cardiovascular risk factors: a systematic review and meta-analysis. Obes Rev 2016;17: 1001-1011.
4. Kritchevsky SB, Beavers KM, Miller ME, Shea MK, Houston DK, Kitzman DW, et al. Intentional weight loss and all-cause mortality: a meta-analysis of randomized clinical trials. PLoS One 2015;10: e0121993.
5. Harrington M, Gibson S, Cottrell RC. A review and meta-analysis of the effect of weight loss on all-cause mortality risk. Nutr Res Rev 2009;22: 93-108.
6. Fryar CD, Carroll MD, Ogden CL. Prevalence of overweight, obesity, and extreme obesity among adults: United States, trends 1960–1962 through 2009–2010. https://www.cdc.gov/nchs/data/hestat/obesity_adult_09_10/obesity_adult_09_10.htm. Accessed 16 June 2017.
7. Menke A, Casagrande S, Geiss L, Cowie CC. Prevalence of and Trends in Diabetes Among Adults in the United States, 1988-2012. JAMA 2015;314: 1021-1029.
8. National Center for Health Statistics. National Health and Nutrition Examination Survey. https://www.cdc.gov/nchs/nhanes/index.htm. Assessed 16 June 2017
9. Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation 2014;129: S102-138.
10. Stevens J, Truesdale KP, McClain JE, Cai J. The definition of weight maintenance. Int J Obes (Lond) 2006;30: 391-399.
11. Wannamethee SG, Shaper AG, Whincup PH, Walker M. Characteristics of older men who lose weight intentionally or unintentionally. Am J Epidemiol 2000;151: 667-675.
12. Connor Gorber S, Tremblay M, Moher D, Gorber B. A comparison of direct vs. self-report measures for assessing height, weight and body mass index: a systematic review. Obes Rev 2007;8: 307-326.
13. Seijo M, Minckas N, Cormick G, Comande D, Ciapponi A, Belizan JM. Comparison of self-reported and directly measured weight and height among women of reproductive age: a systematic review and meta-analysis. Acta Obstet Gynecol Scand 2018.
14. Stevens J, Keil JE, Waid LR, Gazes PC. Accuracy of current, 4-year, and 28-year self-reported body weight in an elderly population. Am J Epidemiol 1990;132: 1156-1163.
15. Kraschnewski JL, Boan J, Esposito J, Sherwood NE, Lehman EB, Kephart DK, et al. Long-term weight loss maintenance in the United States. Int J Obes (Lond) 2010;34: 1644-1654.
16. Yaemsiri S, Slining MM, Agarwal SK. Perceived weight status, overweight diagnosis, and weight control among US adults: the NHANES 2003-2008 Study. Int J Obes (Lond) 2011;35: 1063-1070.
17. Nicklas JM, Huskey KW, Davis RB, Wee CC. Successful weight loss among obese U.S. adults. Am J Prev Med 2012;42: 481-485.
18. Weiss EC, Galuska DA, Kettel Khan L, Gillespie C, Serdula MK. Weight regain in U.S. adults who experienced substantial weight loss, 1999-2002. Am J Prev Med 2007;33: 34-40.